Hystery (haha) of Hysterectomies
The first recorded vaginal hysterectomy was in the 2nd Century AD, performed by Soranus of Epheus for a prolapsed uterus. During the 18th Century, there was a 90% mortality rate for women who underwent hysterectomies. And in 1843, Dr. Clay performed the first successful subtotal hysterectomy in Manchester, England, although the poor women died several days after her surgery. In 1847, chloroform was introduced as an anesthesia during surgeries, but due to it’s toxicity, surgeries had to be performed within one hour. In 1853, Dr. Burnham of Massachusetts, performed the first successful abdominal subtotal hysterectomy with a surviving patient. Interestingly enough, it was somewhat accidental: while excising an ovarian cyst, his patient vomited (there was no anesthesia) and the force of her vomiting pushed the uterus out of the abdominal incision. Unable to return the uterus to the cavity, Dr. Burnham was forced to remove it. During his next 15 hysterectomies, he only lost 3 patients. In 1878, German doctor, Freund, introduced the first reproducible “simple” hysterectomy; and in 1898, Austrian doctor, Schauta and his student Wertheim, performed the first successful radical hysterectomy for uterine cancer. In 1929, Dr. Richardson of the United States performed the first total abdominal hysterectomy. France introduced the gynecological laparoscopic surgery in the1940s; however, the first laparoscopic hysterectomy was not performed until 1988 by Dr. Reich. The DaVinci robotic laparascopic system was approved by the FDA in 2000 and the first robotic laparoscopic hysterectomy was performed in 2005.
Some statisticians believe that 300 out of every 100,000 women will undergo a hysterectomy for a variety of medical reasons. And some say 1/3 of American women will have a hysterectomy by age 60. Some insurance companies consider hysterectomies an elective procedure and may not cover the costs of the surgery…
Different types of Hysterectomies
A partial hysterectomy (aka supracervial or subtotal) is when the doctor only removes the uterus, leaving the cervix intact.
A total hysterectomy is when the doctor removes the uterus and cervix.
A radical hysterectomy is when the doctor removes the uterus, the cervix, the tissues around the uterus, and the top part of the vagina. This is generally performed only when cancer is present.
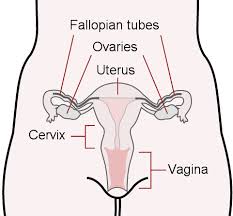
What about the ovaries? If the doctor decides to remove an ovary (which is optional), it’s called an oophorectomy. If both ovaries are removed, it’s considered a bilateral oophorectomy. Salpingo-oophorectomy is the removal of the ovary and its adjacent Fallopian tube.
Hysterectomies can be performed traditionally (a large incision through the abdomen) or minimally invasive (laparoscopy, robotic laparoscopy, or even through an incision in the vaginal canal).
What to Expect Afterward
If a patient undergoes a traditional, open hysterectomy, she can expect more than a 3-day stay in the hospital. She is also expected to return to normal daily activities in 4-8 weeks. Most patients are ordered to avoid sex and lifting heavy objects for approximately 6 weeks.
If a patient undergoes a minimally invasive hysterectomy, she could be home as early as 2-3 days. They are also expected to return to their normal daily activities in 3-4 weeks. Some patients recover in 1-2 weeks with the vaginal hysterectomy. Most are ordered to avoid sex and lifting heavy objects for approximately 6 weeks.
If the patient had both ovaries removed during the procedure, their body will be thrown into instant and irreversible menopause. They may suffer from the usual horror stories: hot flashes, night sweats, lack of sexual desire, hair loss, vaginal dryness, etc.
If the ovaries were not removed, they may still enter menopause earlier than they would have prior to surgery.
How Does It Cure Endometriosis?
It does not. There is no cure.
A hysterectomy may ease our suffering because we no longer have monthly periods. But if the surgeon accidentally leaves behind any Endometriosis implants or cells within our bodies, it is likely our symptoms will return. Many, MANY EndoWarriors claim relief from their Endo symptoms after having hysterectomies. However, many also have had their symptoms returned afterward.
After a hysterectomy, especially if both ovaries were removed, a patient may start hormone replacement therapy (HRT). Most HRT regimens include estrogen. It is believed that Endometriosis feeds and grows off of estrogen…so if any cells remain inside, they may continue to grow, despite having undergone a hysterectomy…and the symptoms may return. Even during cases of excisions where all visible lesions have been excised (even by an expert surgeon), Endometriosis may still recur.
There simply is no proof that a hysterectomy is a guarantee of Endometriosis relief. It is a hope, a relief; however, not a cure.
Potential Risks
In additional to the normal risks associated with all surgeries, some patients who have hysterectomies may have the following future medical problems: blood clots; urinary incontinence; vaginal prolapse (part of the vagina coming out of the body); fistula formation (a connection between the vagina and bladder); and chronic pain.
Alternatives to Hysterectomy
Many EndoWarriors have opted to follow a more natural course of treatment. Altered diets, supplements and herbs, essential oils, sitz baths, massages, and many more. They strive to maintain a hormonal balance and control their Endometriosis symptoms and growths and avoid surgery. There are many webpages and books available on these subjects.
When the time comes for me to talk to my doctor about a hysterectomy, I’m not sure what I’ll do. Honestly : no clue. But I do feel far more educated today than I did yesterday!
(Updated December 28, 2020)
Resources:
AdvancedGyn.com
Biomed.brown.edu
Department of Health : New York
Ethesis.helsinki.fi
HysterectomyRx
*Sunday is “Reader’s Choice” where my readers, friends, and family get to suggest a topic. Today’s topic came from Pamela Benenati-Chandler, “I would like to know more about Endometriosis and recommended hysterectomy??” This topic appealed to me since it also may be in my very near future. So research began! Again, I am a layman. I do not hold any college degrees, nor mastery of knowledge. Please take what I say with a grain of salt. If curious, do your own research 😉 Validate my writings. Or challenge them. And ALWAYS feel free to consult with your physician. Always. Yours ~ Lisa




One thought on “Readers Choice : Hysterectomies & Endo”