A bird’s eye view of the pelvic floor muscles
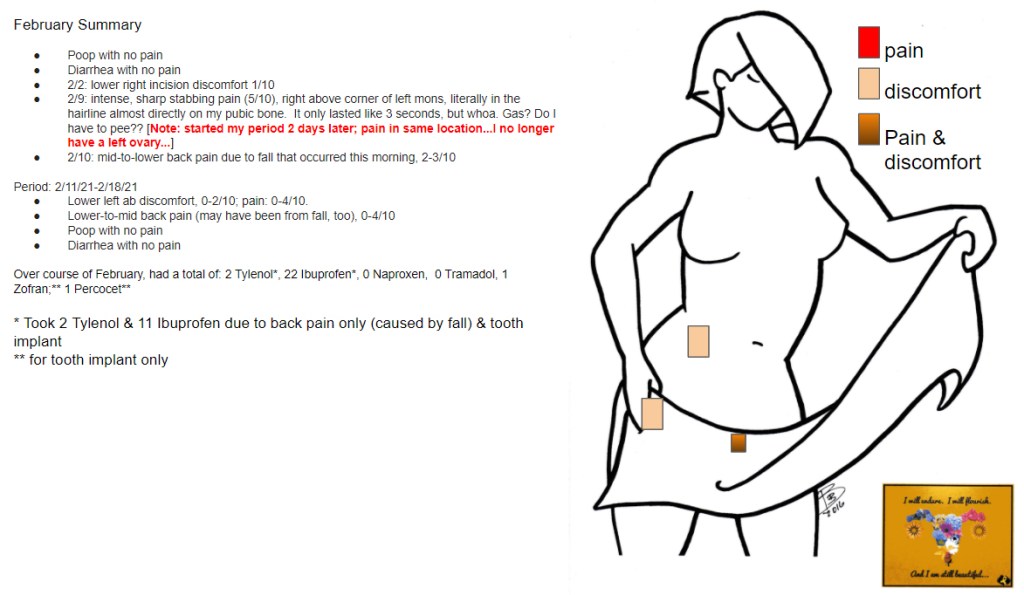
Have you heard of pelvic floor dysfunction? I hadn’t; not before meeting women who suffer from it. And I’d never heard of a pelvic floor before that, either. We’re going to focus today on pelvic floor dysfunction in women (although men can get it). But what is it?
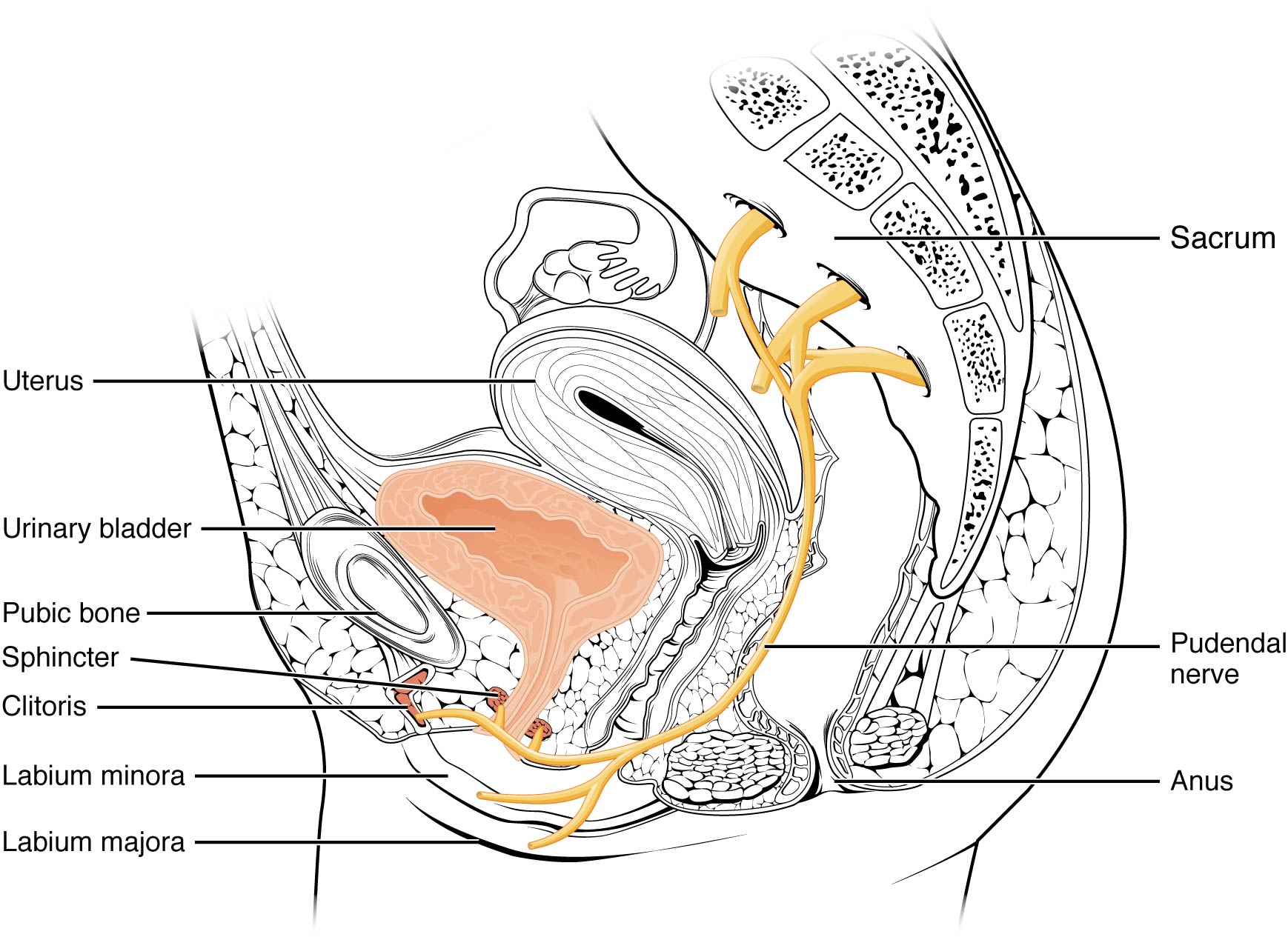
The pelvic floor is made up of a lot of little muscles, nerves, and tissues all working together for your body to function. Imagine it as a tightly-woven basket at the underside of your pelvis, sweeping from front to back, and side to side. Not only does it support the organs of the pelvis, but it also wraps around the urethra, rectum, and vagina. When these muscles, nerves, and tissues stop working properly (they are too tense or too lax), it’s called pelvic floor dysfunction. It can cause pain and difficulty with urination, defecation, intercourse, and lower back pain.
Continue reading →