
What an incredible Journey leading up to my fifth surgery! Covid-19 postponed my surgery date by a week but, just in the nick of time, California’s governor lifted some lockdown restrictions that allowed for my surgery to move back to it’s original date of May 13, 2020. Today, June 10, 2020, marks one month since my surgery! Already! I am overjoyed with the results and the skilled hands of my surgeons.

The Hospital
Due to safety measures of C-19, my Mum wasn’t able to join me for this surgery and recovery. My husband was only able to drop me off at the curb of the hospital and I had to walk in alone. I didn’t see him again until he was picking me up to take me home. It was a surreal experience. No piano player to greet me in the lobby and two checkpoints to pass with Covid questions, but I knew I was in good hands and the time passed super-quickly.
As usual, the hospital staff were incredibly kind and compassionate. There were even a few familiar faces from prior surgeries. Scripps Memorial Hospital in La Jolla really does make me feel like a part of the family. And it made me feel far less alone while I waited.
The two-hour time window between check-in and surgery flew by. Forms, questions, answers, IVs, talks with surgeon, talks with the anesthesiologist, talks with OR nurses, talks with prep nurses. Before I knew it, it was time to roll on back.
One of my favorite questions to ask before each surgery: “What music will we listen to in the OR?” The option for me to choose is always given, but I default to the surgeon’s choice. This time (and always?): “Chill” station. Perfect. So the last thing I remember before taking that surgical nap: being wheeled into the OR, introduced to the rest of the OR staff, and after a few laughs and getting positioned on the operating table, a gentle whoosh of fluid through my veins (I can’t remember for the life of me what the anesthesioligst said before injecting the magic juice), and waking up in recovery.
I always wake up freezing cold. So the nurses were wonderful and turned up the heat on my air-blanket. I’ve GOT to get one of those for home. Ha! Then I fell back asleep, woke up later, and began the transition from naptime to going home.
The timeline? I arrived at the hospital at 5:15am, and was wheeled to the OR around 7:20am. Surgery began at 7:50am and the report was dictated immediately after at 9:47am. My surgeon called my husband at 10:20am to discuss what he found. The nurse called Jim around 11:47am to let him know I’d be ready to go home soon, and we made it home at 1:00pm.
The Surgery

Get on to the nitty-gritty already! I’ll include images of my official op report, followed by my (untrained) laymen explanation. All the learning!
Dr. Mel Kurtulus was my surgeon and Dr. Chandra Spring-Robinson was the Assistant Surgeon. Both are from San Diego Women’s Health and I cannot speak highly enough of them, both for my surgical care and for my regular gynecological needs and Endometriosis symptom management.
If you recall, I had a bowel surgery in 2018 and have rocked a 2-inch vertical scar beneath my belly button. In order to avoid any complications with scars, my surgeon decided to open a port and take a peek under the hood through an incision beneath my left rib cage rather than his usual route (through my belly button). So he took a quick look, realized that the belly button was free and clear of any adhesions, and opened up the rest of the ports: I have incisions on the right torso, my belly button, and two on my left torso.
Once properly situated, strapped in, and stirruped to the OR table, a foley catheter was placed inside my bladder. Through the belly button incision, they pumped my abdomen full of 3 liters of CO2 gas (this helps plump up the belly so they can see clearly inside).

The uterus appeared normal (please remember they suspect I have Adenomyosis, which is not visible as it hides within the uterine muscles).
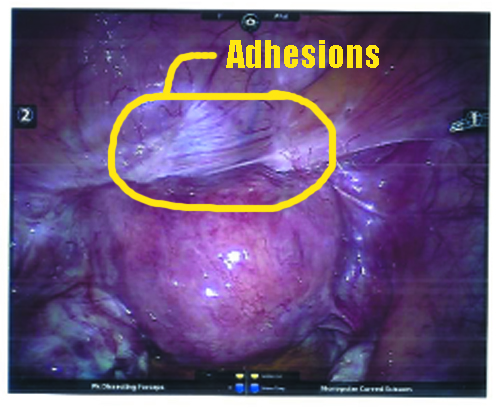
My bladder was stuck to my uterus and pinned there by adhesions. In the photo, it looks very spider-webby.
The right ovary had a cyst which they assumed was a benign cyst.
The left ovary was pulled and stuck to the left side of my pelvic wall by adhesions. It also had a cyst present.
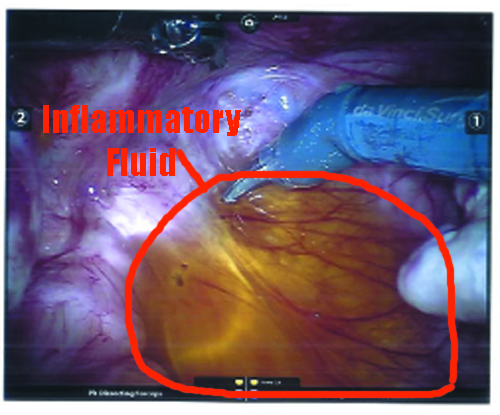
Not mentioned in the report, but is visible in the photographs and was discussed at my post-op meeting, was the yellow-tinged inflammatory fluid in my pelvis. It was at the bottom of my pelvis, just floating around as loose fluid. If you’ll recall a few months ago, my ultrasound technician found “loose fluid” in the area of my intestines. I was advised that this is “inflammatory fluid” and is normal to find in instances of leaking cysts, endometriosis, and adhesions. The fluid was removed during surgery.

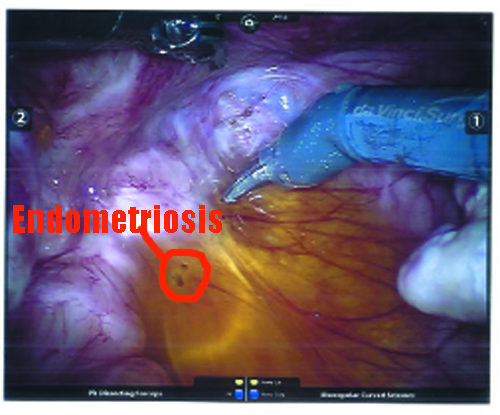
Endometriosis lesions were found on the outside of my bladder, as well as the right round ligament, the cul-de-sac (also called the Pouch of Douglas), the left round ligament, the left paracolic gutter, and on the sigmoid colon. All of the lesions (except for the sigmoid colon) were excised and packaged up for pathology.

Due to the closeness of the left ureter to the endometriosis lesions near my left ovarian fossa (the little cavity of the pelvis where an ovary sits) and the stuck left ovary against the pelvic wall, my surgeon took great care to keep the left ureter safe from any surgical damage. The left ovary and its cyst were completely removed. We had previously agreed to remove my left ovary due to ongoing pain and it proving to be a problem-child (for lack of a better term) discovered during previous surgeries.

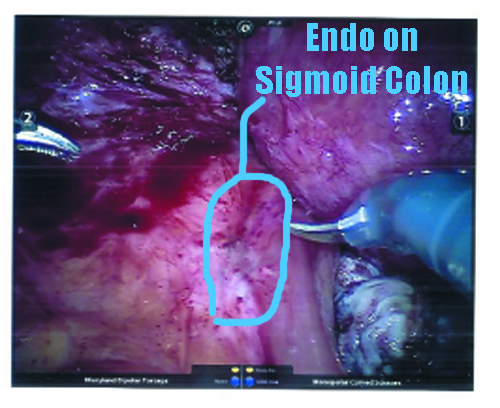
Now, back to the guts. On my distal sigmoid colon, he found a patch of Endometriosis, which he notes as “a deep penetrating cluster of endometriosis lesion.” In my post-op appointment, he classified it as a nodule of Endometriosis, and said it looked like Deep Infiltrating Endometriosis to him. Unfortunately, due to the high risks involved in cutting that deeply into the intestine without a full bowel prep and a colo-rectal surgeon on hand, he took note (and photographs) of its positioning and opted not to remove the nodule. More on this will be addressed in “The Plan” section below.
According to an April 2003 study published in Human Reproduction, Deep Infiltrating Endometriosis (also referred to as DIE) is described as “…a particular form of endometriosis that penetrates greater than 5mm under the peritoneal surface [citation omitted]. These lesions are considered very active and are strongly associated with pelvic pain symptoms [citation omitted].” Brigham and Women’s Hospital in Boston, Massachusetts says that DIE is a rare occurrence, showing up in only 1-5% of women who have Endometriosis.

He then removed the cyst on my right ovary and was able to save the ovary.
He thoroughly checked the rest of my pelvic cavity and found no further Endometriosis. He freed all adhesions and restored any wonky anatomy to its rightful place.
Before closing me up, a bag was placed inside my pelvic cavity, Lefty was tossed inside the pouch, and all was pulled out of my body. YAY! Good riddance! All of the CO2 gas was expelled from my pelvic cavity. And I mean ALL of it. I had ZERO occurence of post-laparoscopy shoulder pain due to any remaining CO2 gas. NONE. Dr. Kurtulus and I refer to it as the “Lisa Special,” where extra time and care is taken to make sure it’s all out. He does it for all of his patients and one day I hope he publishes the importance of taking extra time and effort to teach other surgeons. With all the gas gone, I was sealed up.

Also, per tradition, he took a look inside my bladder in search of any signs of Endometriosis or Interstitial Cystitis or anything else that should not be there. Clean as a whistle and beautifully pink.
Another surgery wrapped up. All involved are skilled at what they do. And this has been THE EASIEST recovery yet.
Photographs
Since not everyone will want to look at my fascinating insides, I’ve embedded the surgery photos at the bottom of this blog entry. Scroll down if you’re curious!
But here’s a one-month progression of my belly healing up after surgery (contains some close-ups of incisions). If you don’t want to watch it, just scroll down a little further to the next section. Although this slideshow only focuses on several days (the entire first week, then once a week after that), I actually do have pictures from every day while healing. Believe it or not, they do help me when I forget if the bandaid lasted that long, or if that incision oozed, or if “this” looks normal. I go back to prior surgery photos often. And I recommend it for your personal notes.
Pathology Results
The pathologist, Dr. Kurt Mathews, found that all of the lesions were Endometriosis. Dr. Mathews also identified the right ovarian cyst as a benign cyst and the left ovarian ovary as a hemorrhagic corpus luteal cyst: both cysts were normal; neither was an an Endometrioma. Which is great news to me. Maybe my body will behave, eh?
The Bills
As of June 29, 2020, I am still waiting to receive most of the insurance Estimate of Benefits/ itemization and confirmed payments:
- The hospital: $89,775.18
- This includes the OR and pathology lab fees, medications, supplies, and equipment
- The surgeon: $5,373.00
- The assistant surgeon: $1,368.00
- The anesthesiologist: Pending
- The pathologist: $671.26
- This is payment to the pathologist for the tissue examination.
- My co-pay: $500
- TOTAL: $97,687.44 (pending bills still need to be added as of 6/10/20)
The Plan
My post-op went very well and all of my questions and concerns were addressed. I have a follow-up consultation on September 1, 2020. At that future visit, we will discuss any remaining symptoms of pain or discomfort. As of today (June 10, 2020), I’ve had no recurrent pre-op symptoms. Any discomfort or pain that I am having is due to the healing process of surgery.
We will monitor my post-op bowel pain. When I poop I once more have the feeling of glass shards running through my guts, which wasn’t present before surgery. Most likely, the intestines are still healing and adjusting from the laparoscopy. I was told that this generally fades a few weeks to months after surgery.
Dr. Kurtulus had already had a private conversation with my colo-rectal surgeon about the Endometriosis nodule on my sigmoid colon. If I do decide to go in for another surgery to have that nodule removed, it will likely be very similar to my 2018 bowel resection. Only the small portion where the lesion is embedded would need to be removed. I’ve forwarded the surgery photos and op report to my colo-rectal surgeon, Dr. Matthew Schultzel, for review and discussion. If after the 3-month follow-up I have had any ongoing or new pain in that area, I will have to decide then what to do.
But the plan?
- Wait and see. If any symptoms become unbearable, go in for surgery. Hopefully it never happens. But I am struggling with the mental aspects of accepting that a deep-infiltrating nodule of Endometriosis remains inside my body and is just lying in wait.
- Continue to maintain (and better) my diet, lifestyle, and exercise.
- I will also continue to daily track my diet, symptoms, and any needed pain medication use. And I will bring summaries of those journals to Dr. Kurtulus in September.
- But the biggest part of the plan? Remain positive during all of this.
Comparison to Past Surgeries
Where was Endometriosis found throughout this whole journey? How much did the surgeries cost (even if covered by insurance)? I always like to go back and compare. And, unless otherwise noted, all lesions were excised:
June 30, 2014: 2 incisions; 2.5 cm Endometrioma on left ovary; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located on liver, diaphragm, between bladder and uterus, left ovary, cul-de-sac, and various locations throughout the pelvis; the uterus was adhered to the bladder; peritoneum adhered to the bladder and uterus; left ovary and fallopian tube obliterated and adhered to adnexa; cul-de-sac obliterated and covered in adhesions; and bowel was adhered to left side of pelvic wall. The liver and diaphragm Endometriosis was not removed. Total cost: approximately $71,000. Surgeon: Dr. Mel Kurtulus
September 21, 2016: 4 incisions; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located on diaphragm, sigmoid colon serosa, right ureter, left side of uterus, various locations throughout the pelvis; adhesions were found throughout the pelvic compartment; uterus was adhered to bowels in several areas; both ovaries and fallopian tubes were clustered and stuck together; right ovary was adhered to backside of uterus; uterus adhered to right side of pelvic wall; and extensive scar tissue on bowel and backside of uterus. The liver Endometriosis lesion had disappeared and the diaphragm Endometriosis was not removed. Total cost: $93,472. Surgeon: Dr. Mel Kurtulus
July 18, 2018: 4 incisions; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located in cul-de-sac, small intestine, near the sigmoid colon, left ovary, fallopian tubes; the tubes were inflamed and covered in disease and were both fallopian tubes were surgically removed; adhesions were found on and near the sigmoid colon, fallopian tubes, and bladder; the sigmoid colon was adhered to left pelvic wall and the bladder was stuck to my uterus. The diaphragm Endometriosis had disappeared. The small intestine Endometriosis was not removed. Total cost: $121,669.50. Surgeon: Dr. Mel Kurtulus
November 26, 2018: 5 incisions; 2cm Endometrioma on left ovary; Endometriosis lesions located on terminal ileum (small/large intestine), cecum, appendix, cul-de-sac, both uterosacral ligaments, near the bladder, and on both ovaries; adhesions had formed on the left side of my pelvic wall, my left ovary was stuck to the left side of my pelvic wall, and my bladder was adhered to uterus; a portion of my small intestine, large intestine, cecum and appendix were all removed, totaling approximately 7 inches during the bowel resection portion of this tag-team surgery; microscopic Endometriosis was found on appendix and cecum, as well as large intestine. Total cost: $235,429.60. Surgeons: Dr. Matthew Schultzel and Dr. Mel Kurtulus
May 13, 2020: 4 incisions; 3cm hemorrhagic corpus luteum cyst on left ovary; 1.2cm benign cyst on right ovary; Endometriosis lesions were found on the outside of my bladder, right round ligament, the cul-de-sac, left round ligament, left paracolic gutter, and deeply-embedded on my sigmoid colon; my bladder was adhered to my uterus, the left ovary was adhered to the left pelvic wall; and my left ovary and adnexa were removed completely. The sigmoid colon Endometriosis nodule was not removed. Total cost: Pending. Surgeons: Dr. Mel Kurtulus and Dr. Chandra Spring-Robinson
The Recovery
Let me start by saying this has been the easiest recovery yet! In a future post, I’ll share my itemized recovery day-by-day journal (I write down EVERYTHING from the second I’m home to four weeks out). And my husband has offered to help so we can compare it to previous surgery recoveries…as well as identify factors that may have made a difference in this time. So, please stay tuned for that separate blog entry.
During the four-weeks following surgery, I had ZERO shoulder pain from CO2 gas (thanks to Dr. Kurtulus and the “Lisa Special”!). And I took ZERO opiates and only two NSAIDs! TWO! I’m so amazed!!! Every day was an experience and journey. So, please stay tuned for the day-by-day breakdown, triumphs, pitfalls, setbacks, and “Today I could do this” entries which I’ll publish as soon as I’ve transcribed it. If I typed those here, this blog would go on FOREVER (and it’s already sooo long)!
Update 7/4/20: it’s been nearly 8 weeks since surgery. I have VERY little surgery pain. If I do, it’s mostly discomfort of low levels. If I overdo things, the discomfort can become pain, but it fades quickly. I DO HOWEVER still have pain when I poop: gut-splitting pain. And I’m curious how my July period will be. June’s period had 2 days of intense pre-op pain on the lower left side. We’ll see!
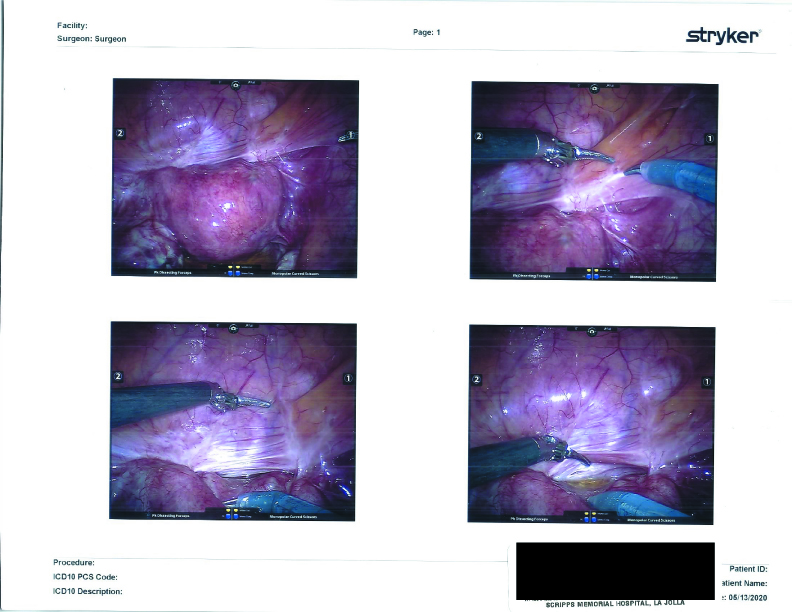
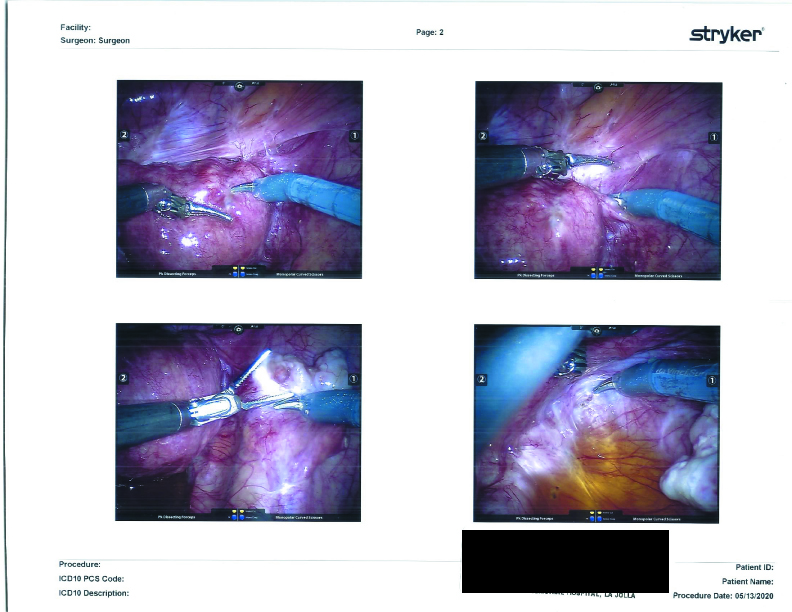
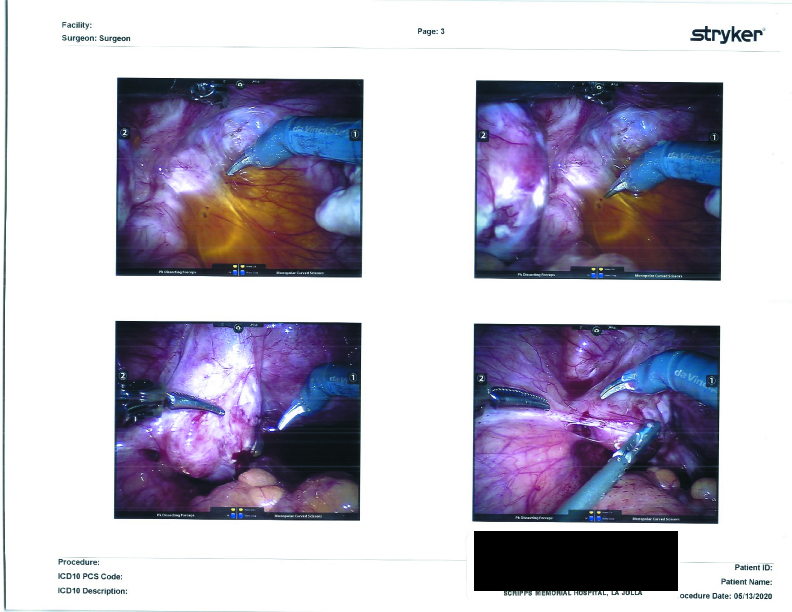
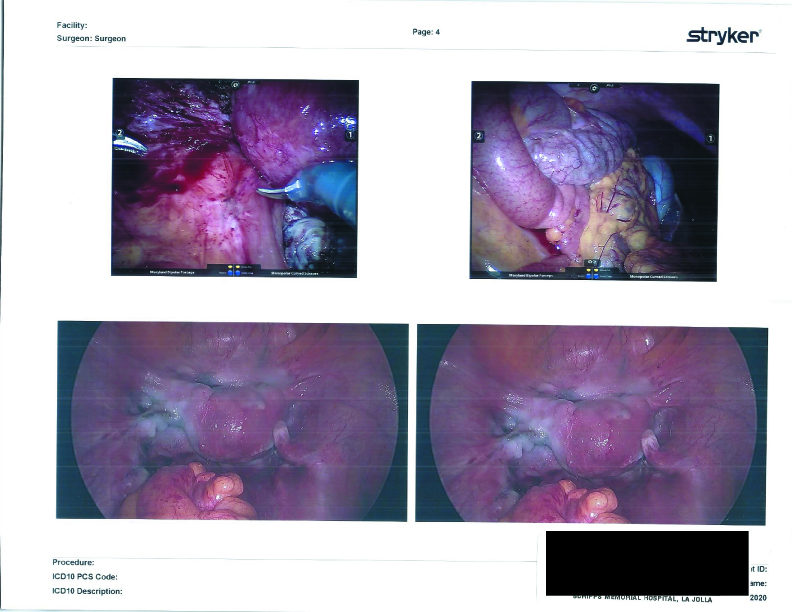
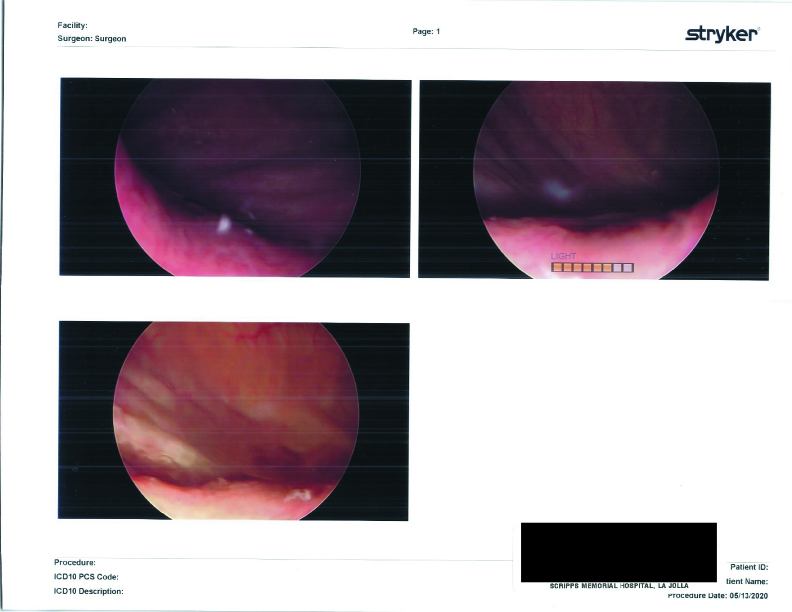
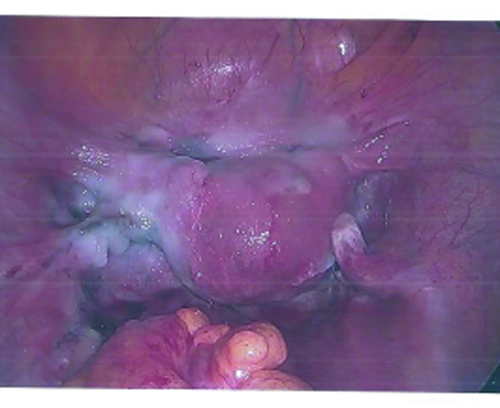
Surgical Photographs
As promised here are the surgery photographs! Please be aware that the scans are low quality; the Endo on the colon is MUCH more visible, almost a dark purple blotch on the hard printouts. If I get higher-quality scans, I’ll be sure to update these. You can click on them for a larger image.
Did you actually read all the way to the end? OMG. You’re amazing!! Not only is this blog meant as a tool to help others with their surgeries, recoveries, etc., but it’s absolutely a tool for myself: If I need to have another surgery, I can come back to these notes and refresh on what I may need or expect. So, thank you for enduring an incredibly lengthy blog entry!
And if you have your own upcoming surgery, I hope it provides long-lasting relief, that it is a easy recovery, and please feel free to reach out to me if you ever need anything.
*Updated 7/4/20*



Thank you for sharing your experience! I am only in the stage where I suspect I have endometriosis, but I find it very reassuring to read about your experience and know how surgery/surgeries can go! Best wishes for easy healing!
LikeLiked by 3 people
And yes, I read it all! : )
LikeLiked by 2 people
Yaaaaayyyyy!
LikeLiked by 1 person
Thank you! And best of luck to you on your journey for answers! I’m always here if you need anything!
LikeLiked by 1 person
Thank you for sharing 💛 rest up and I send you love and light
LikeLiked by 2 people