A friend asked me to look up any connections between Endometriosis and Cesarean Sections. So, here we go. Lots of science in this one! Some studies show that less than 1% of women who undergo a cesarean section end up developing incisional Endometriosis (Endometriosis in or along the c-section scar). However, that tiny little 1% number has a staggering amount of studies involving a lot of women who suffer from this form of Endo.
What is a Cesarean Section?
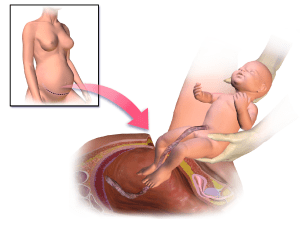
A cesarean section (aka a c-section) is a surgery performed to deliver a baby through an incision in the mother’s uterus and abdomen, rather than vaginally. C-sections can be performed by choice or out of medical necessity (physical abnormalities or other health issues or there is a complication with the pregnancy). Also, if a woman has delivered before by c-section, the chances of a successful vaginal delivery may decrease, and subsequent c-sections may be recommended.
The Atlantic reported that many women in many countries around the world are coerced into have a cesarean section instead of a natural birth due to time constraints, while others bribe their physicians to perform a c-section in order to secure a bed in an overcrowded hospital. Some refer to c-sections as an “economic machine,” one physician can perform up to eight procedures in a day.
Why is this a concern to women or the medical community? Women should be able to choose to give birth naturally or via c-section. Some women have no choice. The concern arises out of an increasing number reports of non-medical emergency cesarean sections; and the coinciding increasing reports of women developing Endometriosis and endometriomas inside or adjacent to their scarring.
How does Endo form in a scar?
There are a few theories about how Endometriosis and/or endometriomas can form inside or adjacent to a surgical scar. The first being surgical transplantation. In simple terms: it was picked up somewhere along in the abdominal cavity during surgery and literally transplanted (either by surgical tools, sutures, fluids, etc.) onto the abdominal wall. As the scar heals closed, the cells continue to grow and may begin to manifest symptoms. Another theory is migration. The endometriosis cells and implants are transferred through the lymphatic or venous systems and deposited to various sites around the body.
It’s just like everything else we hear about Endometriosis : the medical community isn’t sure how or why it happens, but there are many, many documented cases of it happening. Thankfully, procedures are in place to help diagnose, excise, and treat these implants. And, if we are lucky, we will one day have the medical understanding and wide-spread acceptance of a cause, and a cure.
Diagnosis & Treatment
As you will read in the studies below, the gold standard in diagnosis is the usual : surgical excision. Many studies report a lack of relapse/recurrence after the mass is excised. Others report a small recurrence, with a repeat surgical procedure. Some even suggest ongoing medical referrals and the usual medical treatments of hormones and/or hormone suppressants.
The lesson of today’s research and blog (in case you don’t want to read through the following studies) is : if you have an abdominal scar which now has a lump, that may or may not cause you pain, please go have it checked out…Hell, even if it isn’t growing alongside a scar. Lumps can be very, very bad; maybe even cancerous. They can also be harmless, but…why take a risk? Just go have it looked at…
Studies
In 1980, the Obstetrics & Gynecology journal published a study which reviewed the cases of 17 women over five years. These women all had scar Endometriosis and 71% of them had previously undergone a hysterotomy (i.e. cesarean section). Each complained of pain and swelling of their surgical scars around the time of their periods. It turns out 24% of them were diagnosed with Endometriosis after undergoing excision surgery and biopsies.
A study published in 1996 states that 0.1% of women who have had a cesarean section suffer from an endometrioma in the incisional scar; and 25% of those women have pelvic Endometriosis. The endometrioma pain may worsen with coughing or movement. This study reviewed the cases of four women with incisional endometriomas: all four women complained of a painful lump (2 were misdiagnosed as hernias) and the lumps were each removed. Biopsies of each of the four lumps were confirmed as Endometriosis. It concluded that misdiagnoses of abdominal lumps needs to be addressed; as many lumps being operated on as hernias may, in fact, be Endometriosis.
In 1999, seven women were studied over a two year period who shared symptoms of a painful abdominal lump. All of them had some sort of abdominal surgery (six cesareans, two laparoscopies, and one hysterectomy), and only one had a prior Endometriosis diagnosis. Their symptoms began anywhere from six months to 10 years post-surgery. Diagnostic tests and imaging studies were performed prior to surgery; the masses were surgically removed and biopsied. Half of these women were found to have an endometrioma. One patient even had a recurrence, which was excised 22 months later.
In 1999, a Korean study documented the findings of Endometriosis of a cesarean scar turning into clear cell carcinoma. Cancer. It is considered to be the first of its kind. The 54-year-old patient had been complaining of a growing mass over the past three months. Over 20 years ago, she had undergone two prior cesarean sections. Imaging studies revealed the mass, and it was surgically excised. A biopsy showed that it was clear cell carcinoma, with a focus on Endometriosis. She then received six weeks of radiotherapy.
A study published in 2000 reviewed 10 cases of women with incisional Endometriosis. All 10 of these women had a history of a cesarean sections, and had reported a slow growth of a “painful lump” along their incision scar. Some even had symptom changes during their menstrual cycles. Each woman had this lump surgically removed. This study has hopes of raising physician awareness of a patient’s medical history, specifically for Endometriosis, prior to performing a cesarean section.
A European study published in 2002 covered two women who complained of growing, painful masses along their cesarean scars. Each described their pain as strongest just before they started their periods. Each woman underwent excision surgery and the lump was biopsied: Endometriosis. The author is worried that this phenomena is more common that has been previously thought, and these painful lumps need to be surgically excised.
Another 2002 European study examined six women, ages 20-34 years old who had undergone previous cesarean sections. Each of these women had complaints of a painful lump along their surgical scar, some have been complaining of the pain for seven years! The lumps were surgically removed and biopsied and were classified as endometriomas. The authors of this study suggest that the surgical incisions of cesarean patients need to be “cleaned thoroughly and irrigated vigorously with high-jet saline solution before closure.”
A Brazilian study published in 2002 reviewed 199 patients who complained of pelvic pain from 1998 to 2000. Of those 199, 116 agreed to have a diagnostic laparoscopy performed. Of those women with chronic pelvic pain, 67% of them had prior cesarean sections, 52% suffered from adhesions, 34% were diagnosed with Endometriosis, 32% had pelvic inflammatory disease, 11% suffered from pelvic varices, and 7% had leiomyoma. The study concluded the cesarean sections may be a factor in chronic pelvic pain complaints and may become a growing public health concern.
A study published in 2005 reviewed 11 cases of women who also complained of a painful lump along a previous surgical scar. This lump also increased in size during their menstrual cycles. The difference in this study as opposed to the 2000 study was these 11 women had various scars: cesarean, episiotomy, or even a vaginal cuff surgery; it was not limited to only cesarean sections. Among these women, the onset of their symptoms occurred at various stages after their surgeries: some women complained of these symptoms 2 years after their surgery; some 11 years. The women all had their painful lumps removed and biopsied: each one was positive as Endometriosis. This study concludes that incisional Endometriosis seem to be common in women who have undergone a cesarean section, or other gynecological surgery, and warns that caution needs to be practiced during any surgery to avoid the surgical transplantation of endometriosis cells.
A study published in 2006 reviewed 15 patients who were post-cesarean section. Sixty-six percent of the women complained of abdominal pain during their menstrual cycles. The first symptoms’ appearance ranged between 11 months to five years. Each patient underwent a surgery, and any lesions discovered along the scar tissue were removed. This study noted, “[t]he surgical treatment has to be sufficiently wide to avoid all recurrence. No means of prevention has proved its efficiency.” In other words, remove more than just the lesion/implant just to be safe…and prevention is not guaranteed…
In 2012, a study was published in The Journal of Obstetrics and Gynecology Research that discussed the medical histories of 18 patients who were diagnosed with Endometriosis of surgical scars from 2008 to 2010. Each had reported the slow growth and swelling of a painful mass in or near their incision scars (for some, the pain worsened during their periods). Imaging studies were captured on all patients and surgeries were performed to remove the masses. Each mass came back from biopsies as abdominal wall Endometriosis. The women underwent two years of follow-up examinations with no events of recurrence.
A study published last year focused on pelvic adhesions in women who had cesarean sections more than a year ago. In total, 308 women underwent transvaginal and transabdominal ultrasounds and it was discovered that 45% (nearly half) suffered from pelvic adhesions, and 79 also had adhesions in their vesicouterine pouch. It was discovered that “[t]here was a significant association between the presence of anterior compartment adhesions and chronic pelvic pain.” Although not focusing on Endometriosis, this study did help show that adhesions may develop after any surgery or internal trauma, and those adhesions may cause significant pain.
A 2015 published study focused on a 27-year-old woman who had complaints of a painful mass for the past 2 years. She had a previous cesarean section and the mass grew adjacent to her scar, and would increase in size. The mass was brown to black in color and was also visible on an ultrasound. The clinical diagnosis said it could haven been either a suture granuloma, hematoma, melanoma and desmoid tumor. The patient underwent fine needle aspiration cytology, aka FNAC (which is when a skinny needle is inserted and a small sample of tissue is removed and examined) and the tissue was biopsied and found to be Endometriosis. She then underwent surgery to excise the mass, which was confirmed as Endometriosis in pathology tests. She did not have any Endometriosis located anywhere else, nor did her symptoms return. The authors believe that the FNAC procedure could be a valuable tool in pre-operative diagnoses of abdominal wall Endometriosis.
A 2015 Indian study reported that a 32-year-old woman had a c-section six months ago, and now had a lump which had been growing in size and increasing in pain, especially during her menstrual cycle, over the past three to four months. Initial diagnoses noted it may have been a dermoid cyst, a foreign body, a lipoma, or just an abscess. After an ultrasound, the pre-operative diagnosis remained a “foreign body granuloma.” She was given a local anesthetic, and the mass was removed and biopsied. Endometriosis… The authors believe that the cause of this incisional Endometriosis was surgical transplantation, although she had no history of pelvic Endometriosis. They stress, that “it is strongly recommended that the used sponge should be discarded immediately after cleaning the uterine cavity, the suture material used for uterus should not be reused while closing abdominal wall, and finally the surgical area should be cleaned thoroughly and irrigated with saline solution before closure.” They further note that although imaging studies and FNAC techniques may help in a pre-operative diagnosis, surgical excision is still the best way to diagnosis and treat abdominal wall Endometriosis.
A study published on February 18, 2015, studied 17 cases of abdominal endometriosis over a 12-year period. Each study participant had a previous abdominal surgery. The 17 cases commonly shared complaints of a painful mass that worsened and grew during their periods (see Figure 1). Their painful symptoms began anywhere from 1-15 years after their surgeries. Each mass was surgically removed, along with a margin of adjacent tissue in order to avoid missing some cells and allowing for recurrence (unfortunately, one woman did have a relapse and underwent a second excision surgery). And 100% of the biopsies came back as Endometriosis. One. Hundred. Percent. But how many of these women had Endometriosis elsewhere in their bodies : only 14%. As a side note, the FNAC procedure was used prior to surgery in these women as well (see above-referenced study) and again was noted as a possible diagnostic aid.

An April 2016 study published in the International Surgery Journal discussed a 24-year-old woman who had complaints of a painful bump for 2 months. She had two prior C-sections, one 4 years prior and another 2 years ago. It was surgically removed and biopsied and found to be Endometriosis.
A July 2016 study was about three women who suffered from Endometriosis in their scars.
- A 40-year-old woman had two prior cesarean sections and had been complaining of a lump near her bellybutton along her c-section scar for the past two years. It became painful and swollen during her period. It was excised and biopsied, confirmed as Endometriosis – and her symptoms faded.
- A 36-year-old woman also had two prior cesarean sections. Her pain began six years ago, over her c-section scar, and felt like a burning/pricking sensation beneath her skin and would begin and end with her period. When it was removed, her surgeons discovered it was filled with “chocolate-covered fluid” (sound familiar?) and was invading her skin and muscle tissue. It was biopsied, and … Endometriosis. She had routine follow-up visits for the next two years : still symptom-free.
- A 33-year-old woman had a c-section two years ago. She developed a brown lump on her scar, which became painful during her periods. It was excised, and confirmed to be Endometriosis. Years later, still symptom-free.
A December 2016 study was of a 27-year-old woman who had three previous c-sections. For about a year, she’d had a lump in her belly button which caused her “constant pain” that also flared up during her periods and had clear to cloudy discharge at times. Upon physical examination, it caused her pain when it was touched. An ultrasound was performed and it appeared to be a cyst. She underwent an explorative laparoscopy: her uterus was adhered to her abdominal wall, likely due to her previous c-sections and the lump was removed from her umbilicus. Biopsy: confirmed it was Endometriosis.
An article published in January 2017 focused on a woman who had a C-section 10 years ago. She had no previous history of Endometriosis and went to the emergency room because of the development of a painful lump along her stomach, very close to her C-section scar, that she had noticed a few days ago. Interestingly enough: she was on Day 3 of her period. Imaging studies showed a mass, and she underwent an excision procedure. The lump was removed and biopsied and found to be Endometriosis. She has been pain-free since it’s removal. The authors stress that Endometriosis should always be suspected in similar situations, especially if the woman has had a C-section, regardless of the amount of time that has passed between delivery and development of the lump.
An article published in the January 2017 edition of the Journal of Midwifery & Reproductive Health is about a 37-year-old woman who had complained of a painful c-section scar for the past five years (her c-section delivery was six years ago). Her pain and swelling of the scar increased during her period, and was a hard little the rest of the time. She had no prior history of Endometriosis. An ultrasound was completed, which led the physicians to suspect scar Endometriosis. A needle-biopsy was taken of the mass, which confirmed Endometriosis, and the entire mass was removed. The authors stress that physicians take these complaints of pain seriously, conduct an ultrasound and needle-aspiration cytology (needle biopsy) to help lead to a diagnosis and better understanding of what the mass is. They also suggest a complete excision of the mass, plus a 1cm margin of healthy tissue around the mass…although recurrence of the scar Endometriosis is still a possibility, and follow-up examinations should be conducted.
An article published in late January 2017 followed seven women who had developed a mass along their abdominal scars, whether it by hysterectomy, hernia, or c-section. Doctors used the method of fine needle aspiration to biopsy the masses, which pointed toward Endometriosis, and excision surgery was recommended. If you have a mass along your scarring, talk to your doctor. A simple biopsy may yield some answers.
A February 2017 study was about a 32-year-old woman who had a painful lump in her c-section scar (which took place 9 years ago). The lump been around for about 8 years, was painful (moreso during her period), had slowly been getting bigger, and it had begun to turn blue around the area (this study has photographs!). She went to the the emergency room due to the severity of the pain and the alarming blue-tint. The lump measured 10x11cm (roughly 4×4 inches!) and was very painful when touched. Imaging studies confirmed the presence of fluid in the surrounding tissues; they cyst had ruptured. It was surgically removed, confirmed to be an Endometrioma, and it had not returned at the time of her six-month follow-up.
A February 2017 study discusses a 37-year-old woman who had a lump form within her c-section scar, which would occasionally hurt and leak brown fluid when she was on her period. She had a history of three prior cesarean deliveries, and the lump appeared seven months after her last delivery. Palpating her scar revealed a lump approximately 3″ by 1.5″, which had a spot in the center which would leak thick brown good if you pressed around it (no vomiting, please). Surgery was performed and the mass, and surrounding bits and pieces, were excised and biopsied, confirmed to be Endometriosis. Two years after her surgery, there was no recurrence.
A March 2017 article discusses three cases of women who developed Endometriosis in their c-section scars. 1) A 26-year-old woman had two c-sections; the first three years prior and another 8 months prior. She developed a hard, painful, swollen mass in her scar, which would bleed on the first day of her period. It was removed, biopsied, and confirmed as Endometriosis. 2) A 22-year-old woman had a c-section three years prior and now had a reddish, tender bump in her scar; the pain increased during her period. Her physicians suspected scar Endometriosis, removed it, and confirmed their findings through a biopsy. 3) A 30-year-old woman had a c-section performed a year and two months earlier. Her scar actually secreted a discharge, and an ultrasound confirmed a cystic mass within her scar. Her doctors thought it was an abscess, removed it, and a biopsy proved it was Endometriosis.
The Journal of Obstetrics and Gynaecology Canada published a 2017 article, with photographs, of a 36-year-old woman who developed a bump in her lower-right abdomen after a c-section. It was just to the right of her surgical scar. It was excised and biopsied and confirmed to be Endometriosis; she had no reports of recurrence six weeks after her surgery.
HJOG.org published a study in October of 2017 about a 28-year-old woman who had a c-section and developed a painful lump in her scar four months after the procedure. She’d dealt with the pain for the last four years. During her period, the lump became very painful and swollen. Based on her complaints and imaging studies, surgery was performed to excise the mass. A biopsy of the lump confirmed it was, indeed, Endometriosis and the patient had no further issues at the time of her post-op follow-up.
A 35-year-old woman was the focus of March 2018 study. She presented with a painful lump in her c-section scar that she had for the past two years. She had no other pain or symptoms. She had an ultrasound and an MRI done and it was decided to remove the lump surgically. It was fully excised, with a wide margin of healthy tissue surrounding it also cut out. And a biopsy confirmed Endometriosis. She had no relapse or recurrent symptoms once she recovered.
In April of 2018, the International Journal of Reproduction, Contraception, Obstetrics & Gynecology published a study about a 31-year-old woman who complained of a bump beneath her c-section scar for the past three years. It was painful and the bump discharged a “greenish colored fluid” during the time of her periods. She had a history of three past c-section surgeries, the last one was five years prior. The lump itself (the full study has photographs!) appeared to be a large brownish-purple blog on her skin. The lump was removed (along with a margin of healthy tissue surrounding it) and sent for biopsy. The biopsy confirmed the post-operative diagnosis of scar Endometriosis. She had no recurrence at the time of her follow-up examinations. The authors theorized that the rise of scar endometriosis cases may be in direct correlation to the increase of cesarean sections being performed. They urge the medical community to consider a diagnosis of scar endometriosis in patients who complain of lumps in scars, especially in those who have had pelvic surgery.
A July 6, 2018, case report in the Journal of Endometriosis and Pelvic Pain Disorders follows a 43-year-old woman who had a painful nodule in her c-section. The bump had grown over the past two years, and it increased in size during her periods (which were also painful). The nodule was surgically removed and her symptoms diminished. Unfortunately, the abstract doesn’t go into any biopsy reports but points to a suspected endometrioma.
In February 2019, a study was published in Medicine Today after 5 years of analyzing medical records of various patients from a Bangladesh hospital. Eight patients had prior c-sections and all 8 had Endometriosis develop in their c-section scars. The common complaint? A hard mass under their incision scar. Three of the women complained of constant pain at the mass-site. One said her mass grew during her period. And time period between c-sections and lump development: from 16 months to just over 5 years. All 8 women had their lumps removed; all were confirmed as Endometriosis during biopsy. Even more stunning? None of these 8 women had pelvic endometriosis. And after a five-year follow, none of them had any recurrent symptoms.
Another February 2019 study followed two women who had undergone c-sections. A 36-year-old woman had complaints of lower abdominal pain, cramping, and the pain had gotten worse over the past several months. The pain was so intense that she was “no longer able…to function” with daily tasks, etc. A physical exam found the hard lump in her c-section scar. A CT scan confirmed the presence of the mass and it was surgically removed; a biopsy confirmed Endometriosis. Two months after surgery, she had no recurrent symptoms. A 40-year-old woman also had a c-section several years prior and had complaints of abdominal pain. Her pain, however, was to her left abdominal muscles, away from the c-section scar. Her physician had treated her with birth control pills and GnRH agonists; her symptoms did not fade. A CT scan found the mass near her left rectus muscles and it was excised and biopsied: Endometriosis. Two months later she was still symptom-free.
An August 2019 study in MOJ Clinical & Medical Case Reports is of a 28-year-old woman who had a painful swelling for the past six years at her c-section scar, which began three months after her c-section delivery. An ultrasound found a small mass along the scarring and it was suspected she had scar Endometriosis. She underwent excision surgery for the mass and pathology confirmed it was Endometriosis. Six months after that surgery, there was no recurrence.
Cureus journal published a January 2021 study of a 45-year-old woman who had had a c-section two years prior to her doctor appointment. Eight months ago, she noticed a swelling mass on her right side. It had gotten progressively gotten larger as the eight months passed, most noticeably when she was on her period. The lump was mildly painful, but was controlled with NSAIDs. She had no other symptoms or concerns, other than the growing lump on her right side near her c-section scar. A hard mass could be felt during a physical examination and a CT scan showed a large 17x15x10cm (that’s nearly 7x6x4 inches!) mass. They guessed it was an abdominal wall Endometrioma, as it was seated in the abdominal muscles and had no other involvement with organs or structures. The mass was excised in surgery and three months later, she had no recurrence. Pathology confirmed their suspicions.
A March 2021 study published in Experimental & Therapeutic Medicine was of a 29-year-old woman who had previously had a c-section two years prior. She had also a prior diagnosis of pelvic Endometriosis and recurrent cysts on her ovaries. Two years after she gave birth, she went to her doctors due to a painful lump next to her c-section scar. Due to her previous diagnosis and subsequent c-section, her doctors suspected cutaneous Endometriosis and excised the mass. Yep; they were correct. One year after the excision, she remained symptom-free.
If you’ve made it to the end of this blog, you have my thanks and admiration. Please, share this if you know of someone having similar complaints. It’s not normal. And it certainly may not be healthy…
I learned so much today. Thank you, MJ. I don’t know if this answers any of your questions, but I sure hope it offers a little bit of insight…
Yours, Lisa
*Updated April 14, 2021*
Resources:
BioMed Central Women’s Health (2015, Article) Endometriosis Node in Gynaecologic Scars: a Study of 17 Patients and the Diagnostic Considerations in Clinical Experience in Tertiary Care Center
Cancer Treatment Centers of America
Case Reports in Obstetrics and Gynecology (Feb. 2017, Article) Cesarean Scar Endometriosis: An Uncommon Surgical Complication on the Rise? Case Report and Literature Review
Cureus (Dec. 2016, Article) A Case of Umbilical Endometriosis: A Villar’s Nodule
Cureus (Feb. 2019, Article) Abdominal Wall Endometriosis: A Case Report
Cureus (Jan. 2021, Article) Giant Abdominal Wall Endometrioma: A Case Report
Diagnostic Cytopathology (Jan. 2017, Abstract) Fine-Needle Aspiration Cytology of Endometriosis
Experimental & Therapeutic Medicine (March 2021, Article) Skin endometriosis: A case report and review of the literature
International Surgery (2002, Abstract) Abdominal Wall Endometrioma After Cesarean Section: a Preventable Complication
Gynecologie, Obstetrique & Fertilite (2006, Abstract) Abdominal Wall Endometriosis after Cesarean Section : Report of Fifteen Cases
The Journal of Reproductive Medicine (2002, Abstract) Cesarean Scar Endometriosis. A Report of Two Cases
The American Surgeon (1996, Abstract) Endometriosis in Abdominal Scars: a Diagnostic Pitfall
Gynecology Obstetrics & Reproductive Medicine (2012, Article) Scar Endometriosis Following Cesarean Section
HJOG.org (2017, Article) Abdominal Wall Endometriosis After Cesarean Section
Indian Journal of Obstetrics & Gynaecology (2015, Article) Cesarean Scar Endometriosis : a Rare Case Report
International Journal of Gynecology Obstetrics (2002, Abstract) Cesarean Section as a Cause of Pelvic Pain
International Journal of Reproduction, Contraception, Obstetrics, and Gynecology – (March 2017, Article) Post Cesarean Scar Endometriosis: Reporting Three Cases
International Journal of Reproduction, Contraception, Obstetrics, and Gynecology – (March 2018, Article) Caesarean Scar Endometriosis: A Case Report
International Journal of Reproduction, Contraception, Obstetrics, and Gynecology – (April 2018, Abstract) Scar Endometriosis: Not a Rarity Now A Day
International Journal of Scientific Study (May 2016, Article) Scar Endometriosis – A Cause for Painful Scar Swelling – A Surgeons Perspective
Journal of Case Reports and Studies (Feb. 2017, Article) Rupture of a Giant Caesarean Scar Endometriosis Nodule – A Case Report and Literature Review
Journal of Endometriosis and Pelvic Pain Disorders (July 2018, Abstract) Scar Endometriosis: A Case Report and Literature Review
Journal of Korean Medical Science (1999, Article) Clear Cell Carcinoma Arising in a Cesarean Section Scar Endometriosis : a Case Report
Journal of Midwifery & Reproductive Health (2017, Article) Incisional Endometriosis: A Rare Case of Painful Scar
Journal of Obstetrics and Gynaecology Canada (2017, Abstract) Abdominal Wall Endometriosis
Medical Journal Armed Forces India (2016, Abstract) Scar Endometriosis: A Series of 3 Case Studies
Medicine Today (2019, Abstract) Scar Endometriosis: Experience of a Surgeon
MOJ Clinical & Medical Case Reports (2019, Article) Cesarean Scar Endometrioma: A Rare Case Report with Literature Review
Obstetrics & Gynecology (1980, Abstract) Scar Endometriosis : A Clinicopathologic Study of 17 Cases
International Surgery Journal (2016, Article) Abdominal Wall Endometriosis: A Case Report and Review of Literature
The American Surgeon (1999, Abstract) Abdominal Wall Endometriosis: a Report of Eight Cases
Journal of Korean Medical Science (1999, Abstract) Clear Cell Carcinoma Arising in a Cesarean Section Scar Endometriosis : a Case Report
Journal of the American College of Surgeons (2000, Abstract) Incisional Endometriosis: an Underappreciated Diagnosis in General Surgery
Journal of Cytology (2015, Article) Scar Endometriosis : Diagnosis by Fine Needle Aspiration
West African Journal of Radiology (2017, Article) Abdominal Wall Endometriosis Ten Years After Surgery
The Journal of Obstetrics and Gynaecology Research (2012, Abstract) Abdominal Wall Endometriosis in the Cesarean Section Surgical Scar : a Potential Diagnostic Pitfall
The Journal of Obstetrics & Gynaecology Research (2005, Abstract) Incisional Endometriosis after Cesarean Section, Episiotomy and Other Gynecologic Procedures
Ultrasound in Obstetrics & Gynecology (2014, Abstract) Prevalence of Pelvic Adhesions on Ultrasound Examination in Women with a History of Cesarean Section
*Sunday is “Reader’s Choice” where my readers, friends, and family get to suggest a topic. Today’s topic came from an my my friend, MJ, who asked, “Lisa, are you aware of any research regarding and links between endo and c sections?” Again, I am a layman. I do not hold any college degrees, nor mastery of knowledge. Please take what I say with a grain of salt. If curious, do your own research 😉 Validate my writings. Or challenge them. And ALWAYS feel free to consult with your physician (or in this case, attorneys). Always. Yours ~ Lisa



Thank you for this.. Very informative.. After a horrible three month long let’s figure out if I have cancer game, my biopsy came back as endometriosis. Didn’t have it before my c section. Guess I’m that lucky 1%! Rather this than cancer I suppose 🙂
LikeLike
SOOOO glad it’s not cancer!!! Were they able to remove the whole bit of Endo from your scar?
LikeLike
Thank you for this, i really feel like ‘what you write it’ and it with me almost 2 year, i go to doctor and they can’t find any wrong with my body, now i pregnant, and maybe i Will Remove it in my next c sectio.
LikeLike