
One of our local EndoSisters has recently been diagnosed with endometrial polyps, something I know absolutely nothing about. So what happens when I know nothing? I research!
What is a polyp?
A polyp is an abnormal overgrowth of tissue, usually a lump, bump, or stalky growth (hence the mushrooms above). They’re most commonly found in the colon, but can be found in the uterus (known as uterine or endometrial polyps), cervix, stomach, throat, nose, and ear canal. There can be just one polyp…or there can be lots.
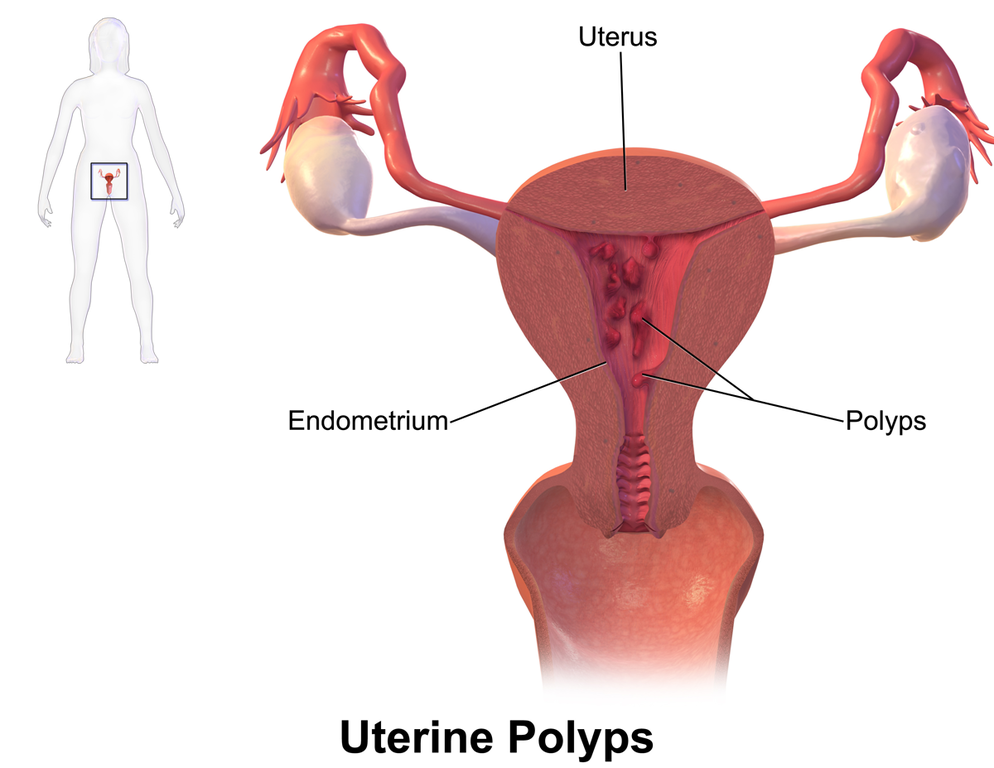
Most polyps are benign (non-cancerous), but there may be a risk that these abnormal cells may develop into cancerous ones. And they can range in size from a sesame seed all the way up to the size of an orange.
Symptoms
Today we’ll be focusing solely on endometrial polyps. Healthline put out a list of symptoms of other polyps. Endometrial polyps only grow along the inside of the uterus, up against the lining.
Before I go into what the symptoms are…I need you to understand that many people do not have any symptoms or complaints – and endometrial polyps may be discovered during routine ultrasounds.

Symptoms of endometrial polyps may include infertility, irregular menstrual bleeding, heavy menstrual bleeding, severe menstrual cramping, bleeding between periods, bleeding after sex, and even vaginal bleeding after menopause. Some women even complain of brown discharge for several days after their periods. This sloughing may occur because polyps may rub the inside of the uterus, causing irritation and exposing blood vessels, which may bleed. Infertility may be caused by polyps blocking the fallopian tubes or even inflamed uterine lining being unable to accept an egg, interfering with the egg and sperm doing their happy dance. Endometrial polyps have been known to interfere with IVF treatments and they should be removed prior to starting IVF treatment.
While we’re talking about vagina, I just want to note that cervical polyps can also cause unusual discharge, bleeding during sex, or even heavier bleeding during periods.
If you suffer from any of these symptoms and don’t know why (or know why, but may suspect something more), have a talk with your doctor. I know a lot of these symptoms mirror symptoms of Endometriosis…Self-advocacy is soooo important.
Causes
Nobody is really certain why polyps develop, although studies are ongoing.
Some factors which may cause your body to create endometrial polyps include inflammation, the presence of a cyst or tumor, excess estrogen (they’re sensitive to estrogen), or even the presence of a foreign object. One theory is that polyps are more likely to form due to the changes brought on by the menstrual cycle and the surge and decline of hormones during that process.
Some people are also more susceptible to growing their very own polyp. People who have birthed children or are over 40 are more likely to develop endometrial polyps. Also, there have been connections found between endometrial polyps and hypertension (high blood pressure), obesity, are taking post-menopausal hormone replacement therapy, who have a family history of Lynch Syndrome or Cowden Syndrome, and those who have taken Tamoxifen.
Tamoxifen is a drug which blocks the body’s receptors so estrogen can’t work it’s magic. People with breast cancer (or at a high risk of developing breast cancer) most often take Tamoxifen; however, it has also been used to treat infertility, bipolar disorder, Riedel’s thyroiditis, retroperitoneal fibrosis, and McCune-Albright syndrome. As a curious side note, studies have shown that Tamoxifen may be linked with stimulating Endometriosis growth since it also thickens the endometrial lining. *runs away*
Diagnosis
As usual, it starts with a verbal medical and symptom history and physical examination. Your doctor may order imaging studies (hysterosalpingogram [a special x-ray using dyes], ultrasound, or CT scans) to visualize any polyps and get a sense of their size and location. However, a regular ultrasound (aka sonogram) and transvaginal ultrasound may not show the polyps and a special “water ultrasound,” called sonohysterogram (or SHG for short), may be required. A saline solution is injected through the cervix into the uterus to expand it a bit and allow for clearer visuals. This allows them a better look around the inside of the uterus. Doctors may also use a hysterscope to peer around the inside of the uterus. This is a small illuminated tube that goes up the vagina and into the uterus. Sounds like fun…
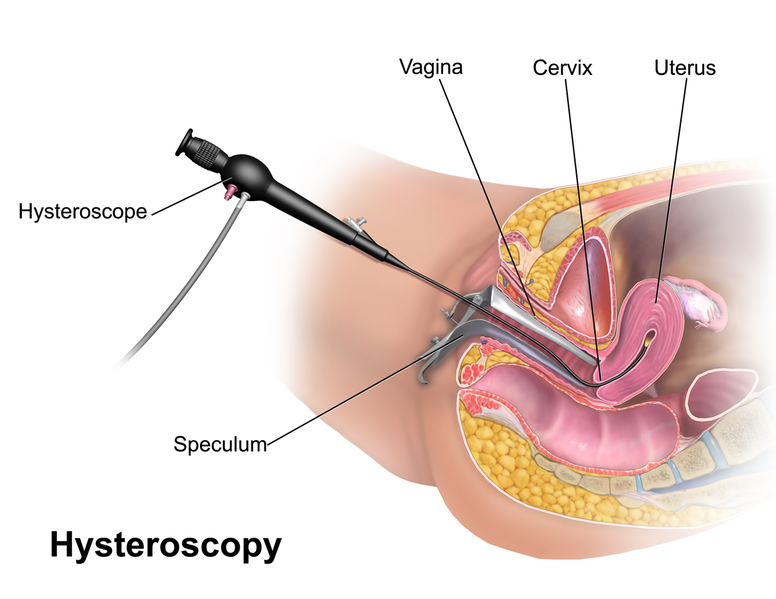
Although these methods may lead your doctor to assume you have polyps, the only way to confirm the diagnosis is by performing a biopsy.
Cancer
Some figures say that 3-5% of polyps can be cancerous or pre-cancerous. So, a doctor will most-likely want to perform a biopsy on any polyp they find, just to confirm it isn’t cancerous. Cancerous polyps are very rare, but chances increase slightly as we age (over 50 and they increase even more). If cancerous endometrial polyps are discovered, your doctor may recommend a hysterectomy.
And, beware – if you have a history of non-cancerous (benign) endometrial polyps, you may have an increased chance of developing uterine cancer. A 2012 study stated that 25% of patients with endometrial cancer had a prior history of some sort of benign endometriail biopsy. So, go in for check-ups. Often.
Treatment
Well, I hate to say this…but what I’ve been reading online for treating endometrial polyps is much of the same of what many of you have known for treating Endometriosis…
Wait and see what happens. Most small polyps that don’t cause any symptoms may just resolve on their own.
To treat symptomatic cervical or endometrial polyps, your doctor may prescribe progestin or even GnRH agonists in an attempt to reduce or eliminate the polyp…say it with me, “Lupron Depot.” It’s like we can’t get away from this drug. AND once the treatment is stopped, the symptoms may return.
If a patient has a history of miscarriages and is trying to conceive or has a family history of cancer, or the the symptoms don’t resolve, her doctor may opt to remove the polyp. The removal of a polyp is a procedure that rolls off the tongue : a polypectomy.
The polyp can be removed with a D&C (dilation & curettage), where the inner lining of the uterus is scraped clean. However, there have been instances where this doesn’t remove a polyp; it just wiggles it around a bit.
Remember that little illuminated tube (hysterscope)? It can be inserted through the vagina and cervix into the uterus, along with itty-bitty tools like scissors or a laser, and the polyp can be cut away. Some surgeons may use a tool known as a resectoscope, which is a tiny tube that (you guessed it) goes up into the uterus. The resectoscope has a tiny wire lasso on the end which allows the surgeon to wrangle and hog-tie the polyp (well, not really), remove it, and send it off to biopsy. Yeehaw!
For those who wish to seek a more natural route of treatment, there are a lot of articles online. If you go this route, please consult with your physician before starting anything! Herbs and supplements that some claim to help relieve symptoms, and reduce or even cure polyps, include: apple cider vinegar, angelica, butcher’s broom, castor oil, cayenne pepper, cinnamon, clove, fenugreek, flax, garlic, ginger, goldenseal, green tea, red raspberry leaf, marshmallow (the herb, not the sugary white smooshy deliciousness), mustard seed, tea tree oil, xanthium, and yellow cedar. Increasing your fiber intake will also help your body flush excess estrogen from the body.
Recurrence
Once a polyp is successfully treated and/or removed, there’s always a chance it will reappear. Statistics show that 15-43% of endometrial polyps reoccur.
Prevention
Want a fighting chance against developing polyps? Unfortunately, endometrial polyps cannot be prevented. If they’re coming, they’re coming. Just take heart knowing they’re really, really common…And do go in for your regular check-ups, including an annual ultrasound, to keep an eye on your insides.
Think you have Endometrial Polyps?
I, again, cannot stress enough to you how you must have a conversation with your physician. It all starts with a talk.
(Updated March 27, 2019)
Resources:
American Journal of Obstetrics & Gynecology – (Abstract; Aug. 2000) Exacerbation of Endometriosis as a Result of Premenopausal Tamoxifen Exposure
Ayurvedic Cure – 9 Top Herbal Remedies for Polyps
Current Opinion in Obstetrics and Gynecology – (Abstract; June 2016) Hysterescopic Polypectomy for Women Undergoing IVF Treatment: When is it Necessary?
Healthline – What are the Symptoms, Types, and Treatments for Polyps?
Ilana Sowter Acupunture Melbourne
International Journal of Clinical and Experimental Pathology – (Article; July 2016) Increased Expression of Nestin and VEGF in Endometrial Polyps: an Immunohistochemical Study
Livestrong – Holistic Treatments for Cervical Polyps
News Medical – Other Uses of Tamoxifen
Search Home Remedy – 6 Best Home Remedies for Polyps
The Center for Menstrual Disorders & Reproductive Choice
The Journal of Obstetrics and Gynecology of India – (Abstract; Aug. 2016) Endometrial Polyps and Subfertility
International Journal of Gynaecology & Obstetrics – (Abstract; April 1994) Endometriosis and Tamoxifen Therapy
Obstetrics & Gynecology – (Abstract; Nov. 2012) Risk Factors for Developing Endometrial Cancer After Benign Endometrial Sampling
Wakemed Health & Hospitals – Learn What to Expect from Endometrial Polyp Removal
~ Again, I am a layman. I do not hold any college degrees, nor mastery of knowledge. Please take what I say with a grain of salt. If curious, do your own research 🙂 Validate my writings. Or challenge them. And ALWAYS feel free to consult with your physician. Always. Yours ~ Lisa





Great post. Thank you for mentioning Cowden Syndrome!
LikeLiked by 2 people
This wass great to read
LikeLike