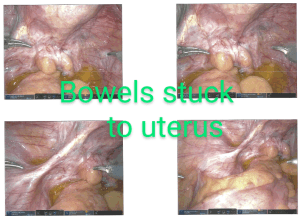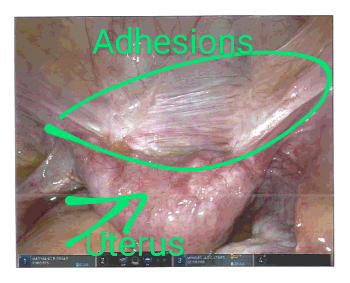
Well, on April 6, 2022, I had my seventh surgery associated with my Endometriosis.
This one was due to several issues:
- Recurrence of pain at my lower left abdomen, lower right abdomen, and some mid-abdomen pain
- The discovery of a fibroid in December 2021
- The ongoing presence of suspected Adenomyosis within my uterine muscles
- The very-real possibility of adhesions (suspected due to passage of time AND my pelvic floor therapy massages)
And this Lucky #7 surgery was to be extra special because we were finally saying goodbye to my uterus (thanks to the fibroid!) I still have my right ovary and my dual cervixes – just no more uterus!
Read more: Lucky Number Seven!The EVE BEFORE
Okay, so having had so much experience with surgeries, I KNOW that being able to try to be in a good place mentally is very important. Scripps Memorial Hospital is about 30 minutes from my house – nobody wants to make that drive at 5am…
Due to Covid, the hospital wasn’t allowing visitors to stay within the walls while I was actually IN surgery, so rather than have my husband miss time from work, I asked my best friend to be my ride. Which meant: SLUMBER PARTY!
We stayed at this wonderful little AirBNB not far from the hospital And had a marvelous night of fun conversation, crazy selfies, geocaching, and R&R. It was epic. Rosie also caught an epic moment o’me waiting for the enema to kick in. If you know: you know!
And? The gate to our AirBNB had a giant “7” painted on it. For no reason.
PRE-OP
Rosie was actually able to stay with me in the hospital up until they wheeled me away to the operating room. And, care to guess where we stayed chatting it up while we waited? Pre-Op Room Number Seven!
We met with my surgeon, Dr. Mel Kurtulus, who just came in for pleasant conversation as I had no questions – but we did have to go through the whole pre-op checklist. We even saw Dr. Spring-Robinson as she walked through the halls off to her own surgery. Flagged her adorable-self over for some pre-op pep talkin’, too. Have I mentioned I love the folks at San Diego Women’s Health?
I even had the same pre-op charge nurse, Karen, that I’ve had at a few other surgeries. She’s awesome.
The anesthesiologist came on by for the pre-op checklist and to answer any questions: one I’ve not had before. So: of course – I had a request…Rather than count me down for my nap, I asked if he would tell m a joke. Ha! He seemed a little perplexed, told me he didn’t know any, but would find one before our time together.
At 7:30am (right on schedule!), I said goodbye to my beloved Rosie.


The op nurse wheeled me down the hall to my operating room, I immediately forgot everyone’s names. But there were about seven nurses/technicians in the op room, the “chill” music station was already going, and there were smiles all around. Once I was properly situated on the operating table, the anesthesiologist began to give me the good cocktail. And the joke:
“How do you tell a male chromosome apart from a female chromosome?”
He then made us wait a moment…giving everyone in the O.R. a chance to guess. And just as my eyelids began to get heavy and I was terrified I was going to miss the punchline, he continued:
“You strip them down to their genes!”
I remember laughing, and asking if he Googled it…YES! He did!
I’m glad I remembered it. It was the last thing I remember before waking up in the recovery room. And the first thing I wrote down when I got home…
The Surgery
Surgery went off without a hitch. It was two-and-one-half hours long from start to finish. And I was in the recovery for a few hours. Rosie was notified via text that I was in the recovery room at 10:16am, and I was in the car with her driving at 12:41pm.
I woke up with four new holes: one on the right, two on the left, and he had to crack my belly button open a bit larger to get my uterus out. We opted to keep my dual cervixes due to the potential for complications with my separated vaginal canal – so through the belly button we went!
During the surgery, Dr. Kurtulus found two suspected Endometriosis lesions on the right side of my pelvis (near the right utersacral ligament and right peritoneum), my remade-sigmoid colon was stuck by scarring to my left pelvic cavity, my uterus was thoroughly scarred to the top of my pelvic cavity, he visualized the fibroid of my uterus, and found some of my bowels were scarred to the backside of my uterus.
Pathology confirmed I indeed did have Adenomyosis. And it found that the two suspected lesions were NOT Endometriosis (just normal tissue); rather it did reveal that the lining of the outside of my uterus was covered in microscopic Endometriosis! It’s called uterine serosa Endometriosis. I learned something new! I wish you could have seen Dr. Kurtulus’ eyes go wide when we read the pathology report together.
I still have my right ovary, which was free of any cysts. And I still have my two cervix. Everything else is gone…in order of their removal: fallopian tubes (2018), left ovary (2020), and uterus (2022).
In my opinion: the likely cause of my pain that led to the surgery:
- Left side pelvic pain: sigmoid colon scarred to left side peritoneum by adhesions;
- Central abdominal pain: Adenomyisis, Fibroid, serosa Endometriosis, bowel scarred to uterus, and uterus scarred to peritoneum by adhesions;
- Right side pelvic pain: perhaps radiating pain or organs pulling due to adhesions.
The photographs of the adhesions and the fibroid amaze me. If you’d like to see them, I’ll include them at the bottom of this blog entry.
It turns out that seven is my surgeon’s lucky number, too!
The gate? The pre-op room? Surgery number seven? And my doc’s favorite number? Oh yeah. I’m taking this all in as a good sign.
The Recovery
This was, by far, the easiest and most pain-free recovery yet.
Here’s some highlights from the notes I took (yep, I take handwritten notes after surgery when I’m home to track pills, pain, sleeping, triumphs, etc.). Why do I write this out? To remind myself if I need a future surgery what the timeline may be – as well as to hopefully help others realize healing takes time…
April 6, 2022
1:00pm: got home and took 2 GasX
3:15pm: I took a Naproxen Sodium for pain (at a 2 out of 10) and was eating pickles by 3:16pm. Aww, the soothing comfort of pickles.
4:34pm: popped a Zofran for nausea, and chased it down with a rice cake. Scrolling through my phone and watching TV made me nauseated.
I had slight CO2 gas pain (1 uot of 10)beneath my right ribs and diaphragm. Every once in a while, that gas pain would hit my right shoulder at a 1 out of 10 pain.
By 7:00pm, I began to feel pain (3 out of 10) where my uterus used to be, but not enough to take a pill.
I took my Klonopin (parasomnia) pill at 8:23 and slept from 9:30pm to 5:55am. I woke up for about an hour and took a little walk sometime during that window. Didn’t toss and turn much (according to my fitbit)
April 7, 2022
6:30am: had pain 2-4 out of 10 and was tender all over. But still managed to walk around. Popped a Naproxen Sodium and a GasX. Thirty minutes later I had a small bout of CO2 pain under my right ribs, but no shoulder pain. Enjoyed a cup of coffee and a rice cake around 9am.
10:30am: I went for a very small, short, and easy walk with Rosie. 0.12 miles; it took 8 minutes. And by the end of it, I was exhausted.
Meals were rice cakes, soups, crackers, some cheese. And Colace (nom nom).
4:00pm: I showered. By myself! And we replaced the bandaids over my incisions and steri-strips.
We went for another walk at 7:17pm. It was shorter (0.05 miles) and longer (12 minutes). When we got back to the house, I popped a GasX and Naproxen Sodium for 1-2 out of 10 pain.
April 8, 2022 (a day of firsts!)
6:20am: out of bed! I slept flat nearly the entire night. Slept for 8 hours and 37 minutes, according to my Fitbit. Spent 49 minutes awake (whether that means fidgeting or wandering the hall; I’m not sure). My husband helped me out of bed, which caused all-incisions to scream a whopping 2 out of 10 pain. It also spurred up minor CO2 pain (3-4 out of 10). I took a Naproxen Sodium, a GasX, an the all-important Colace.
7:00am: I had minor lower back pain (2 out of 10). My husband had to go to work, so our friend Julie came by to keep me company.
8:32am: we went for a walk (0.31 miles; 18 minutes). Nice and slow. And no pain!
It was a celebrate-junk-food day: ice cream and kettle corn!
12:28pm: we went for another small walk of 0.25 miles in 13 minutes. AND – speaking of those triumphs? MY FIRST FART! A doozy! It was massive. And felt great!
5:18pm: My first post-op bowel movement. I used my wee generic squatty potty, didn’t strain. My husband helped me up and off the toilet. Poor man. But YAY for post-op poops!
6:17pm: I took a Naproxen Sodium just to help keep any inflammation at bay
7:03pm: Jim and I went for our last walk of the day: 0.31 miles, 18 minutes. This one had a slight grade/incline – which I felt in my lower back and hips (2 out of 10).
7:35pm: Everyone’s worst nightmare after surgery: THE SNEEZE! I knew it was coming and braced my abdomen with a pillow…but it caused immediate lower left incision pain (6 out of 10)…but was also gone as quickly as it came.
April 9, 2022
8:30am: woke up after 9.5 hours of sleep! Fitbit showed nearly an hour of that was awake (lots of little walks and peeing in the middle of the night, eh?) Popped a Naproxen Sodium forl ower right incision pain (4/10) and a GasX
8:33am: Jim and I wasted time starting the day with a walk! 0.15 miles in 16 minutes with a slight incline. Felt good! Super productive!
3:27pm: Jim and I went on another walk. This one was 0.52 miles in 17 minutes.
5:44pm: Dragged the hubs out on ANOTHER walk! 0.47 miles in 18 minutes. My torso felt tight and itchy. The lower right abdominal area had some discomfort. And I was exhausted.
6:30pm: My first car ride since coming home. We went to our favorite burger joint and I can tell you: I wasn’t ready. Speed bumps=death. Pot holes=death. Hard wooden bench=death. I had pain 6 out of 10 throughout my torso and popped a Naproxen Sodium, GasX, and Colace when we got home at 7:15pm.
April 10, 2022
First of all, let me say: I was able to get off and on the toilet with VERY LITTLE HELP! Finally. It was difficult, and I still needed someone to help me…but…soon: soon I could piss and shit without someone to lift me…BUT I still need help getting in and out of bed…sigh
9:03am: I slept from 9:44pm to 9:03am. Almost 12 hours! Well, Fitbit says I had nearly an hour and 20 minutes awake…probably fidgeting. And walking…
Today the bruises were green. And my skin was so annoyed with the bandaids that I received doctor’s approval to not replace them. Just leave them off and do not pick at the Steri-strips.
9:06am: Naproxen and deep breathing exercises to help try to push out some of that stiffness.
9:16am: small walk with the hubs. Took about 19 minutes, but I didn’t record the distance. But we walked with our morning coffee in hand! Very important detail to have written down, I suppose.
2:32pm: Another walk with Jim. 0.33 miles in 13 minutes. I wasn’t sore, but I was tired.
7:30pm-8:45pm: I eased myself into sitting at the computer. Upright. It was definitely too long. I had right hip soreness and right incision soreness. The entirety of my core was exhausted. I popped a Naproxen and went to bed.
April 11, 2022
Slept for nearly 9 hours. And…I was finally able to get myself in and out of bed! Alone!! With no help. Five days after surgery. In and out of bed. Granted, I waddled around like a turtle stuck on it’s back for a minute, but finally was able to get it out.
6:50am: Took a walk by myself! 0.48 miles, 16 minutes, no pain!
2:35pm: My second poop since surgery. Been a few days…I did have to strain ever so slightly. As a sidenote, I also did have some mild light brown vaginal discharge. But, hey: they did take my uterus, so there’s definitely gonna be some ick coming out. There was no foul odor to the discharge. Once I got myself off the pot, I popped a few stool softeners…
3:30pm: That’s more like it. Poop #3! No need to strain. But I most certainly should be drinking more water…
3:47pm: The flood gates had opened! Poop #4. No straining, but this one did hurt a little bit. All that gut-activity in my newly-renovated pelvic cavity? No more, please.
5:20pm: yet another visit to the restroom. Post-op poo #6. No pain.
6:06pm Poop #7; 6:30pm Poop #8; 6:39pm Poop #9; 6:50pm: Poop #10.
Thankfully that was the last. What a day!
April 12, 2022
Six days after surgery. Another night of great sleep (8.5 hours)
6:50am: solo walk with no pain: 0.35 miles in 11 minutes
Today I was able to sit at the computer 45 minutes at a time with no discomfort. I knew I had to wean myself back into that mode as I’d be going back to work in a little over a week.
10:16am: another walk to help with my sitting-at-computer stiffness. 0.47 miles in 13 minutes. No pain, but got “super tired” at the end.
1:42pm: lots of little walk breaks today to combat the at-the-chair syndrome. 0.34 miles in 10 minutes. A bit of lower back discomfort, but no pain.
1:55pm: since my 45-minute bouts at the computer were going so well, I thought I’d try three hours. Nope. Too long! I was stiff, my belly button was tender. I was exhausted. But: no real pain.
April 13, 2022 (THE ONE WEEK MARK)
Another day of trying to sit at the computer for longer periods of time. Started at 45 minutes, then took a break, then an hour, then another break. Then made it for 2 hours! Then a lunch break. The longest I sat at the computer at the one-week mark was nearly three hours! I had lower back pain and right incision pain. Felt stiff all over. And learned I needed to take a lot of little breaks in between if I meant to honor my body and healing.
April 14, 2022 – April 20, 2022
Sparing you all of the minor details, the recovery continued to inch along. Walks became longer and progressively quicker (although not fast by any definition of the word). One day I did a sort of squat to pick up the remote and was tender at all incision sites. Hot showers and the occasional Naproxen Sodium were still needed after trying to sit at the computer each day. April 14, 2022 was my last Naproxen. And I returned to work on April 21, 2022. Driving, as always after surgery, was a tender endeavor causing all of my incisions to be angry – but not angry enough for medication.
The Bills
Hospital/Op Room/Labs: $155,162.26 billed; insurance paid the contracted amount of $26,534.85. Zero balance.
Pathologist: $587. Insurance denied the claim as it must be submitted directly to the medical group. Medical group could not discuss payment or total amount paid.
Surgeon & Assistant Surgeon: Unknown (medical group would not release amount for privacy reasons)
Anesthesiologist: Unknown (medical group would not release amount for privacy reasons)
Copay: $500 paid out-of-pocket for outpatient surgery
Subsequent bills: $30 paid out-of-pocket for in-hospital labwork. Insurance would not cover since the blood draw was considered a separate and uncovered procedure.
How am I doing now?
It’s been nearly a year. I’ve since crashed into menopause and have started low-dose hormone replacement therapy (Dotti estrogen patch and a testosterone gel). I’ve had zero pain indicative of either Endometriosis or Adenomyosis. It’s been amazing. I have yet to take a pain pill associated with either of those two diseases – and am pleased that (so far…) there’s been not even a hint of Endo’s return – even thought I *am* am estrogen.
I have a follow-up with Dr. Kurtulus in early March. My annual pap takes place in June or July of this year, and I believe an ultrasound around that same time.
I know that every body is different. As is everyone’s Endometriosis. I truly believe that the removal of my uterus was THE BEST THING we could have done in a case like mine: Adenomyosis, a fibroid, and microscopic uterine serosa Endometriosis. Here’s to hoping the Endo continues to stay away.
Why did it take me almost a year to publish this? Simple: I was not ready to look at the photographs and acknowledge the void that is my reproductive system. Having wanted children for so long growing up, then not having any, then realizing I no longer wanted them at my age…yet – still having to SEE no womb? That was the hardest part.
Sex is still painful with deep penetration, but I have to understand that it is my unique anatomy of two cervixes. And my husband and I have learned positions that do and do not facilitate pain-free intercourse.
I know that hysterectomies do not help all people with Endometriosis (and it’s no damn guarantee) – so that’s another reason I’ve been hesitant to share.
And it’s only been a year. Historically, my symptoms return 18-24 months after an excision surgery…but: here’s to hoping.
Never give up.
You are never alone.
And we are all in this together.
The Photos!
(I know not everyone likes to look at surgery photos, so I will always put them down at the end…)
Before we get into the nitty gritty photos: one more fun one from the AirBNB Slumber Party Extravaganza!!!! This – this is my favorite! Even on the even of a (potentially) terrifying event: you MUST find a reason to smile. Be positive. And I’m grateful for my besty!

Okay: on to the fun stuff! The only reproductive things I have left? My cervixes and my right ovary.