On October 21, 2020, I went in for my tag-team surgery with my fellas: Dr. Mel Kurtulus and Dr. Matthew Schultzel. Each had their own specific tasks while they worked together to make sure I was happy, healthy, and well:
- Dr. Matthew Schultzel was going to inspect and remove a portion of my sigmoid colon which had deep-infiltrating Endometriosis (discovered during my May 2020 surgery);
- Dr. Mel Kurtulus was going to peek around inside to see if I had any new Endometriosis growths since May or any scarring or other things that may need to be cleaned up.
If this sounds familiar, we did a similar tag-team effort with these two amazing surgeons back in November of 2018, but for the opposite side of my colon.
The best part? I have had ZERO, zilch, nada, no pre-op pains! The only pain I’ve had since October 21st has been healing from surgery! My November pain journal screamed of the difference in my symptoms and Endometriosis pain!
The Prep
Aw, my favorite: Suprep. Once again, my insurance did not cover the cost of the one liquid 100% necessary for my colo-rectal surgery. BUT if you’re ever in need, please check the manufacturer’s webpage; they often have a coupon! Or look at GoodRX. Any way to save some money!
It was a vicious and never-ending bowel prep this time! I thought Nov. 2018 and my colonoscopy a year later were bad? Oh no! Just know that I poo’d 70 times in approximately 24 hours. If you’ve enjoyed my previous accounting of my experience with a bowel prep, I’ll most certainly be sharing the texts and play-by-play in a future post here.
The Big Day
Due to the Covid-19 pandemic and safety precautions, my husband had to drop me off at the curb of Scripps Memorial Hospital. We shared one quick kiss and tried not to get too dark and foreboding as we wished each other goodbye. And, sadly, I ventured into the hospital alone.
While I waited in the pre-op prep area, the staff were kind enough to allow me to keep my phone with me so I could talk to friends and family before being wheeled away. I also took the opportunity for selfies with my heroes:

Dr. Schultzel and I pre-op 
Dr. Kurtulus and I pre-op
Both surgeons came out to make sure I didn’t have any questions, as well as to review the procedures we had planned. The anesthesiologist, Dr. Jason Ipson, also spent a very long time hearing out my concerns, especially about the shoulder pain that often accompanies laparoscopies. I told him about Dr. Kurtulus’s “Lisa Squeeze” technique, where they try to get out as much of that gas as possible. We also talked about our favorite Halloween candy (his surgery hat was covered in little candy corns) and I learned he loved 100 Grand bars (I ended up mailing some to his office as a thank you later). It was a wonderful way to just relax, share a few laughs, and lighten the mood.
Although it’s my sixth surgery…surgery is still scary. Every time.
I remember being wheeled back into the operating room by my two wonderful OR team nurses, whose names I can’t remember. But they were jovial and friendly and we joked the whole way down the hall. One nurse had fun trying to guess middle names, but guessed mine incorrectly and Dr. Ipson got it on the first try. Maybe he read my chart? Ha.
The last thing I remember before taking that long nap was getting into position on the surgery table, and feeling a cold whoosh through the IV in my right arm.
“Oh! What’s that?” I asked
“That’s the good drugs,” the nurse replied.
Then I woke up in the recovery room. No dramatic countdown. No more jokes. No music. Just I woke up freezing cold until the nurse cranked up my hot-air blanket.
There was a mad dash to find my phone before I was whisked away to the Prebys Cardiovascular Institute‘s 5th floor (surgery recovery unit). All of the staff were amazing and found the phone just as we gave up! Yay! But in the future? I’ll just turn my phone in with the rest of my belongings before I’m all settled in.
What They Found
Let me preface this by saying all the way up to the point where I was told I was going to have to stay in the hospital for a few days, I was nervous and convinced they weren’t going to find anything wrong. Every freakin’ surgery I have these doubts. And every freakin’ surgery I’m proven wrong. Those damn voices…they were wrong again. My pain was real. It had a cause. I wasn’t weak or projecting psychosomatic pain. So, I was drastically relieved when the nurse told me I’d be transferred to Prebys to recover. THEY’D FOUND SOMETHING! I didn’t know what then, but my surgeons told me soon enough.
I remember waking up a little later in my hospital room and pulling my blanket and hospital gown aside. I was both excited and horrified at the incisions. Endometriosis was found and removed. And the overnight stay in the hospital meant they had to remove a portion of my guts. Vindication was mine!
In a nutshell: my body is an overachiever when it comes to Endometriosis:
- Dr. Schultzel confirmed there was a blob of deep-infiltrating Endo on my rectosigmoid junction (where the sigmoid colon meets the rectum).
- Dr. Kurtulus also found Endometriosis lesions
- where my left ovary was (remember, the ovary was removed in May 2020),
- to the left of my sigmoid colon,
- on the exterior of my uterus,
- near my right colon,
- patch of several deep infiltrating Endometriosis lesions in my cul-de-sac,
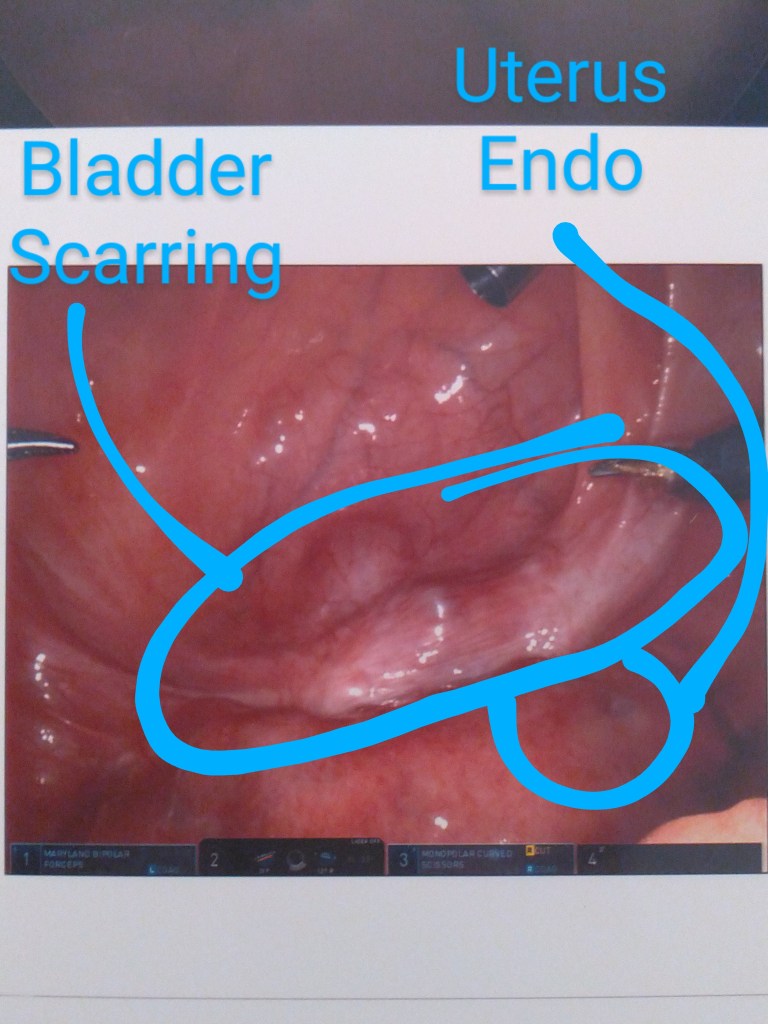
- my bladder was also scarred down to my uterus, yet again, and
- I had a few cysts on my right ovary.
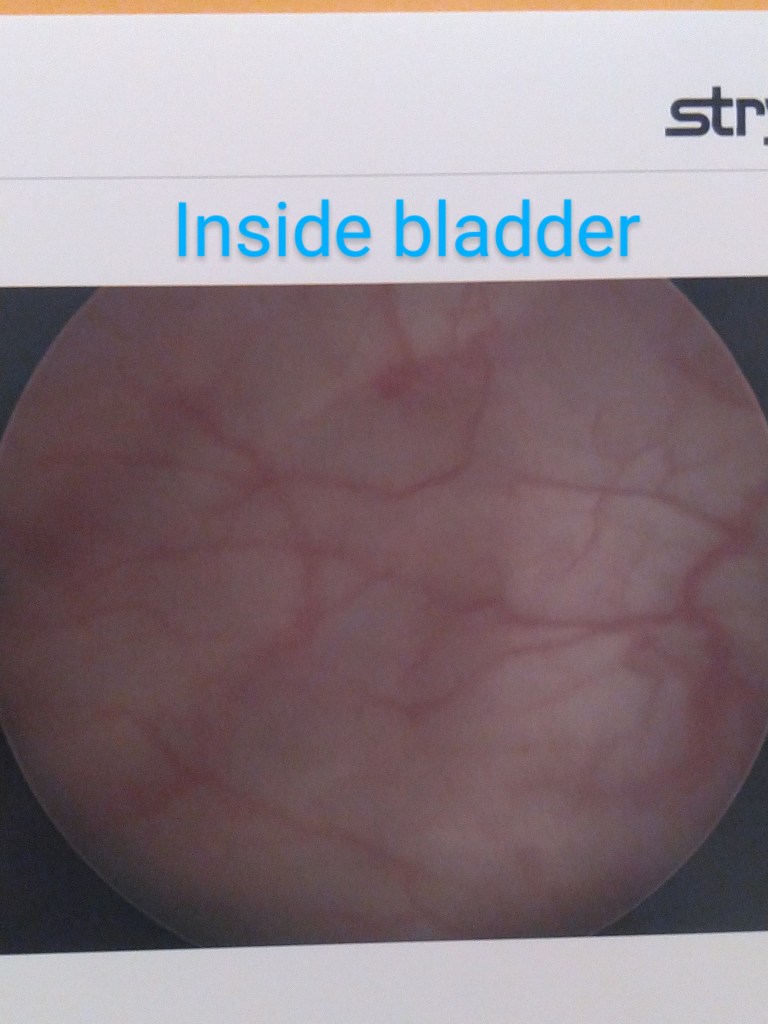
While Dr. Kurtulus was excising the deep infiltrating Endometriosis of my cul-de-sac, one of the lesions was nicked and oozed out the all-too-familiar dark brown liquid similar to a chocolate cyst. So much new growth in new places in just five months. He removed all of the adhesions and lesions he found. The inside of my bladder was clean and perfect.
Dr. Schultzel removed about a 4″ portion of my sigmoid colon, joined the two openings of my guts together, and pulled the little removed section out through an incision near my pubic bone. No need for an ileostomy bag!
The surgery took about 2.5 hours (I think this was my shortest one yet!) But in greater detail, here are excerpts from the op reports:
If you read the highlights of Dr. Schultzel’s report, you may have noticed that…there was a stapler IN MY BUTT! I had to text him to make sure I read that right! HA! Talk about a fun series of texts in the hospital!
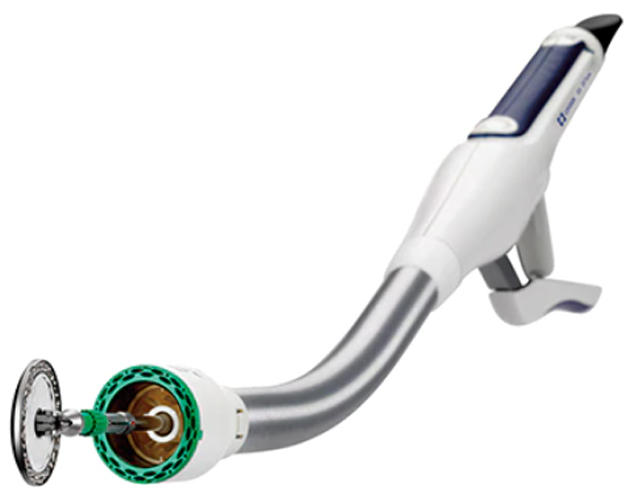
I then became obsessed with researching the type of stapler, the procedure, and how the two sides of the intestines are brought together internally, stapled together, and sealed. An amazing process known as end-to-end anastomosis and I’ve found an animation video that sort of shows what happens during the procedure. But just so we’re clear: I had a big round stapler shoved up my butt! It’s hilarious.
My first thought was like docking spaceships. “Commence Poopchute Docking!”


😉
The Hospital Stay
I was in the hospital from October 21st to October 24th. Of course, my incisions hurt every day. My abdomen was angry. The swelling was a bit big for a few days. And I was helpless. Again, Covid-19 restrictions were in place and I could receive no visitors.
The first night was the absolute worst night I’ve ever had. I’m so grateful Prebys offers private rooms and nobody had to hear me moanin’. The pain was super intense and was given plenty of Dilaudid and Zofran. I had the foley catheter still for the rest of that afternoon/evening and had a lot of short 20- to 30-minute naps. The nurses were amazing at keeping up with my pain medication and making sure I was as comfortable as I could be. And I only had two small instances of minor shoulder pain due to the gas, and it was minimal and not the horrendous pain in the past. I tried to talk-to-text to my cell phone any instances of pain so I could keep my pain tracker accurate…but sometimes I was so high on medication that I have no idea what I intended to say.
For example, can you decipher this lovely gem:
“Laura ab middle pain 6 out of 10 with near lower back pain. You’re welcome or is it back to smashy robber on the back of his head with a cricket bat.” ~10/21/20 @ 11:24pm
October 22nd brought the release of my catheter and the dreaded “get out of bed and walk around” orders. I saw my surgeons daily as they came to check in on me and my progress. When I marveled to Dr. Schultzel about the lack of shoulder/CO2 gas pain, he said it was the Lisa Squeeze and they had three of them pushing on my abdomen to help release the gas from my pelvic cavity. YAY! More surgeons need to diligently get all that damn gas out! It’s so important to an easier recovery! I needed assistance to get in and out of bed, walk around the 5th floor, and get on and off the toilet to pee. The day also brought liquid food, accompanied by a bit of nausea and vomiting. I no longer needed the Dilaudid, but instead the pain was controlled with a cocktail of Gabapentin, Tylenol, Celebrex, Zofran, and the occasional Tramadol. I know a HUGE part of my pain control was the transverse abdominal plane block performed by Schultzel during my surgery. They also gave me Pepcid and a pill to wake my bowels up so I could poop and go home (but that wouldn’t happen for two more days). Walking around the hospital was accomplished with the help of my nurse as she maneuvered my IV stand and I clutched my pillow to my tender abdomen. Four laps around the Prebys 5th floor were made that day.
October 23rd brought a storm of independence! I was able to get in and out of bed alone, as well as walk around by myself as I held my pillow and IV stand. I could even get on and off the toilet to pee alone! The same cocktail regimen continued, including the pill to wake up my guts. This day also brought me my first non-surgeon visitor: Aunt Flo! Yep…my damn period started while I was at the hospital. Ugh. Hospital pads are gigantic! But those boat-pads weren’t going to stop me from walking! I managed to walk around the entire 5th floor wing eight times that day! EIGHT! Woohoo! I wanted my guts to get movin’ so I could go home.
October 24th. I still hadn’t farted or pooped. And by now my guts were just so full of “ugh” it was painful. Lots of walks and the usual medication regimen. And at noon? At noon, I pooped (I completely skipped the farting phase)!!! I victoriously pulled my “Nurse Assistance” cord in the bathroom and nearly yelled “I POOPED!” to the nurse who stuck her head in to check on me! The announcement spread like wildfire, I was given a bit of a soft-food diet (I chose shredded salmon with mashed potatoes), I received my discharge papers, and was home at 7:49pm.
Don’t get me wrong: I was on a lot of pain meds at the hospital. But I was also in a lot of pain. The medication controlled the ongoing pain, but there was a lot of acute pain when I moved or shifted or got out of bed or stretched wrong or yawned or breathed too deeply, etc. It was not an easy ride at all.
The doctors, nurses, nurse’s assistants, cleaning crew, cafeteria staff, and chaplains at Prebys are amazing. This is my second stay there, and they absolutely make you feel comfortable, well-cared for, and part of a family. I even had my favorite nurse (Elizabeth) from two years ago for a few shifts! Epic reunion!
Home Recovery
My seester, Rosie, picked me up from the hospital and took care of me that evening until my husband got home from work. And my wonderful husband stayed with me for an entire week (without pay, I might add!) to take care of me. I was mostly independent with getting out of bed and using the restroom., bt was still 100% restricted from doing anything bendy or reachy or lifty or squatty, etc. Poor Jim had to do everything! I even slid off of the couch while trying to get up and flailed around like a turtle stuck on its back…until my knight-in-shining-bathrobe rescued me 30 seconds later.
I’m shocked. For all of the at-home recovery during October, pain was managed with the occasional Percocet. But in November? All I needed the entire month to manage any post-op pain was Tylenol!
As of today (December 5, 2020), my incision pain is usually a 0-4 on a scale of 1-10 (with 10 being the worst pain ever). No need to even pop a Tylenol for that pain; and if I do need one, it’s only when I’ve done things like I’m doing right now: sitting for several hours. And I still have some sutures that my body is spitting out. They’re snagging on a few things, but for the most part they don’t bother me. I know it will plop out sooner rather than later!
This week all of my post-op restrictions have been lifted (the week of Nov. 29th). I’ve gardened, changed the cat litter, done dishes, washed laundry, and we even had sex! All with zero to minimal pain! It feels good to be an active member of this household again! I can pick up my cats again (20-pound beasties)!
And…again…NO PRE-OP PAIN!!! As usual, we truly hope this is the last surgery I’ll need for Endometriosis. The difference between pre- and post-op is INCREDIBLE!!
Pathology Results
The pathologist confirmed that all of the lesions removed were Endometriosis except for the blob on my sigmoid colon. It’s simply listed as a “defect.” But both of my surgeons have expressed that based on their experience and know-how, they both feel that it was, in fact,deep infiltrating Endometriosis, regardless of the “defect” findings by the pathologist. And based on my complete resolution of symptoms, I have to agree. Not one single bowel movement has hurt. Not one little iota. Oh, and the cysts on my right ovary were found to be corpus luteal cysts.
The Money
Update 12/9/20: my insurance approved the hospital bill! WOOHOO!
As I write this, I’m trying not to freak out (written on 12/5/20).
My insurance has denied the claims based on needing more information from the hospital. I know it will all be okay since the surgeries were both pre-approved by Anthem. But in the meantime, I’m in limbo. I also have no idea what the surgeons and anesthesiologist themselves billed directly to the medical group. I’ve still got to call my medical group to verify the below referrals have been paid. If I do learn of any altered billing, I’ll be sure to update this list.
Per my Anthem Explanation of Benefits, following are the charges for my surgery:
- 10/21/20: $2,250 patient copay for surgery and hospital stay; paid by me;
- 10/21/20: $216,586.84 facilities/hospital stay/hospital care; paid by insurance ;
- 10/21/20: $209.71 hospital care; denied as an out-of-network provider and forwarded to medical group for payment; review/payment pending;
- 10/21/20: $919.31 pathologist examination of tissue; denied and forwarded to medical group for payment; review/payment pending;
- 10/21/20: $943 Dr. Ipson (anesthesiologist); paid by insurance (original bill was $3,240);
- 10/21/20: $8,177 Dr. Schultzel (colo-rectal surgeon); insurance review/payment pending;
- 10/21/20: $1,308 Dr. Burgess (Schultzel’s assistant surgeon); insurance review/payment pending;
- 10/21/20: $860.20 Dr. Kurtulus (endometriosis excision surgeon); paid by insurance (original bill was $1,687);
- 10/22/20: $81.84 hospital care; denied as an out-of-network provider and forwarded to medical group for payment; review/payment pending;
- 10/23/20: $81.84 hospital care; denied as an out-of-network provider and forwarded to medical group for payment; review/payment pending;
- 10/24/20: $153.58 discharge from hospital; denied as an out-of-network provider and forwarded to my medical group to pay the physician; review/payment pending;
- TOTAL: $231,571.32.
I’m always saddened how little my surgeon gets paid for such a life-changing surgery, and always the pathologist makes more. *sigh*
Comparison to Past Surgeries
Here’s one of my favorite parts of my surgery recaps: the great comparison! Where was Endo found in prior surgeries? Has it grown in new places for this surgery?
June 30, 2014: 2 incisions; 2.5 cm Endometrioma on left ovary; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located on liver, diaphragm, between bladder and uterus, left ovary, cul-de-sac, and various locations throughout the pelvis; the uterus was adhered to the bladder; peritoneum adhered to the bladder and uterus; left ovary and fallopian tube obliterated and adhered to adnexa; cul-de-sac obliterated and covered in adhesions; and bowel was adhered to left side of pelvic wall. The liver and diaphragm Endometriosis was not removed. Total cost: approximately $71,000. Surgeon: Dr. Mel Kurtulus
September 21, 2016: 4 incisions; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located on diaphragm, sigmoid colon serosa, right ureter, left side of uterus, various locations throughout the pelvis; adhesions were found throughout the pelvic compartment; uterus was adhered to bowels in several areas; both ovaries and fallopian tubes were clustered and stuck together; right ovary was adhered to backside of uterus; uterus adhered to right side of pelvic wall; and extensive scar tissue on bowel and backside of uterus. The liver Endometriosis lesion had disappeared and the diaphragm Endometriosis was not removed. Total cost: $93,472. Surgeon: Dr. Mel Kurtulus
July 18, 2018: 4 incisions; 2cm hemorrhagic corpus luteum cyst on right ovary; Endometriosis lesions located in cul-de-sac, small intestine, near the sigmoid colon, left ovary, fallopian tubes; the tubes were inflamed and covered in disease and were both fallopian tubes were surgically removed; adhesions were found on and near the sigmoid colon, fallopian tubes, and bladder; the sigmoid colon was adhered to left pelvic wall and the bladder was stuck to my uterus. The diaphragm Endometriosis had disappeared. The small intestine Endometriosis was not removed. Total cost: $121,669.50. Surgeon: Dr. Mel Kurtulus
November 26, 2018: 5 incisions; 2cm Endometrioma on left ovary; Endometriosis lesions located on terminal ileum (small/large intestine), cecum, appendix, cul-de-sac, both uterosacral ligaments, near the bladder, and on both ovaries; adhesions had formed on the left side of my pelvic wall, my left ovary was stuck to the left side of my pelvic wall, and my bladder was adhered to uterus; a portion of my small intestine, large intestine, cecum and appendix were all removed, totaling approximately 7 inches during the bowel resection portion of this tag-team surgery; microscopic Endometriosis was found on appendix and cecum, as well as large intestine. Total cost: $235,429.60. Surgeons: Dr. Matthew Schultzel and Dr. Mel Kurtulus
May 13, 2020: 4 incisions; 3cm hemorrhagic corpus luteum cyst on left ovary; 1.2cm benign cyst on right ovary; Endometriosis lesions were found on the outside of my bladder, right round ligament, the cul-de-sac, left round ligament, left paracolic gutter, and deeply-embedded on my sigmoid colon; my bladder was adhered to my uterus, the left ovary was adhered to the left pelvic wall; and my left ovary and adnexa were removed completely. The sigmoid colon Endometriosis nodule was not removed. Total cost: $97,687.44, but still may have bills pending. Surgeons: Dr. Mel Kurtulus and Dr. Chandra Spring-Robinson
October 21, 2020: 5 incisions; “several” corpus luteal cysts on right ovary; Endometriosis lesions found on outside of uterus, left ovarian fossa (where left ovary used to be), left of my sigmoid colon, on the rectosigmoid junction (DIE), in the cul-de-sac (DIE), near the right colon; and bladder was scarred and held down against uterus. Total cost: $231,571.32, but still may have bills pending. Surgeons: Dr. Matthew Schultzel and Dr. Mel Kurtulus.
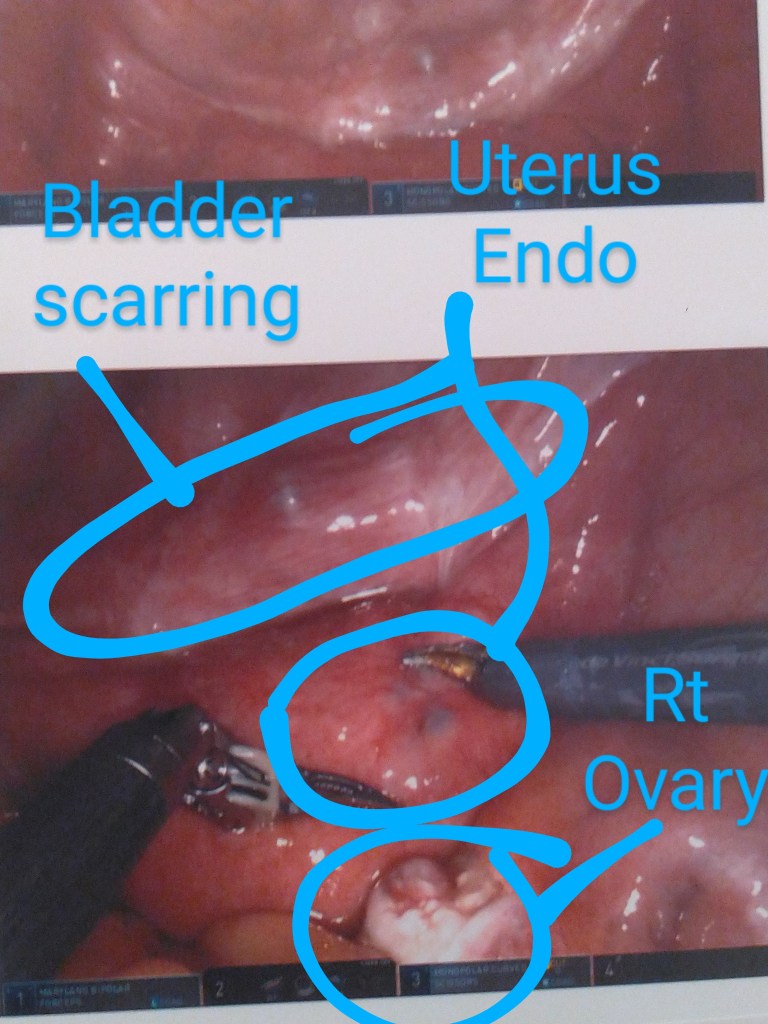
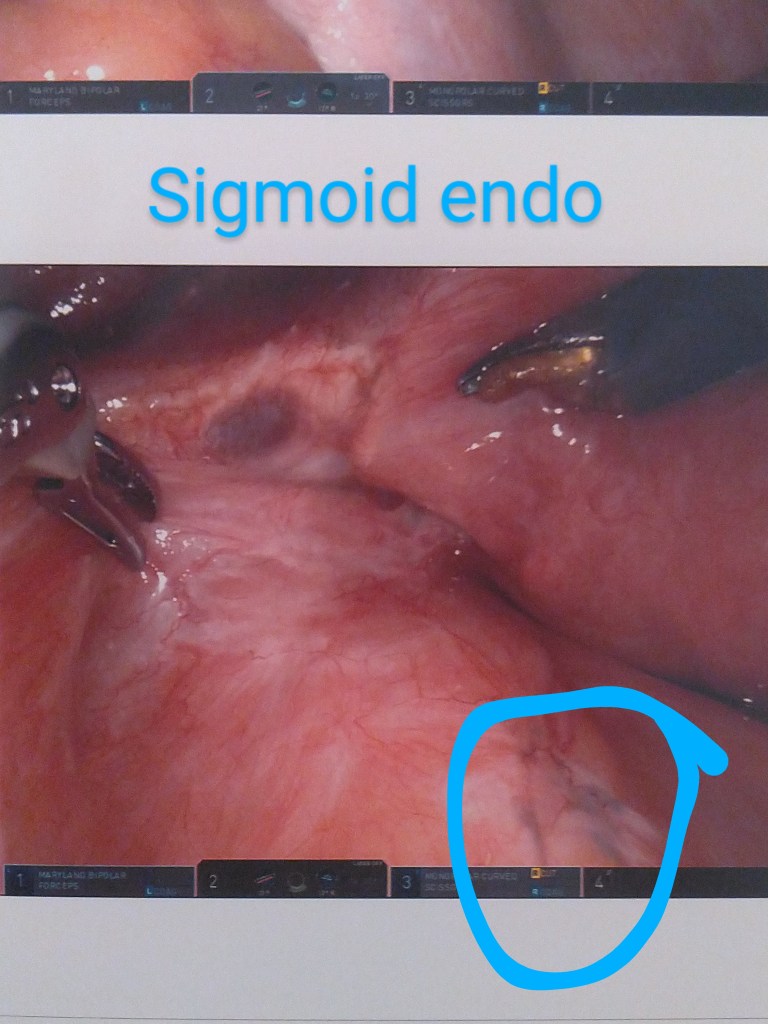
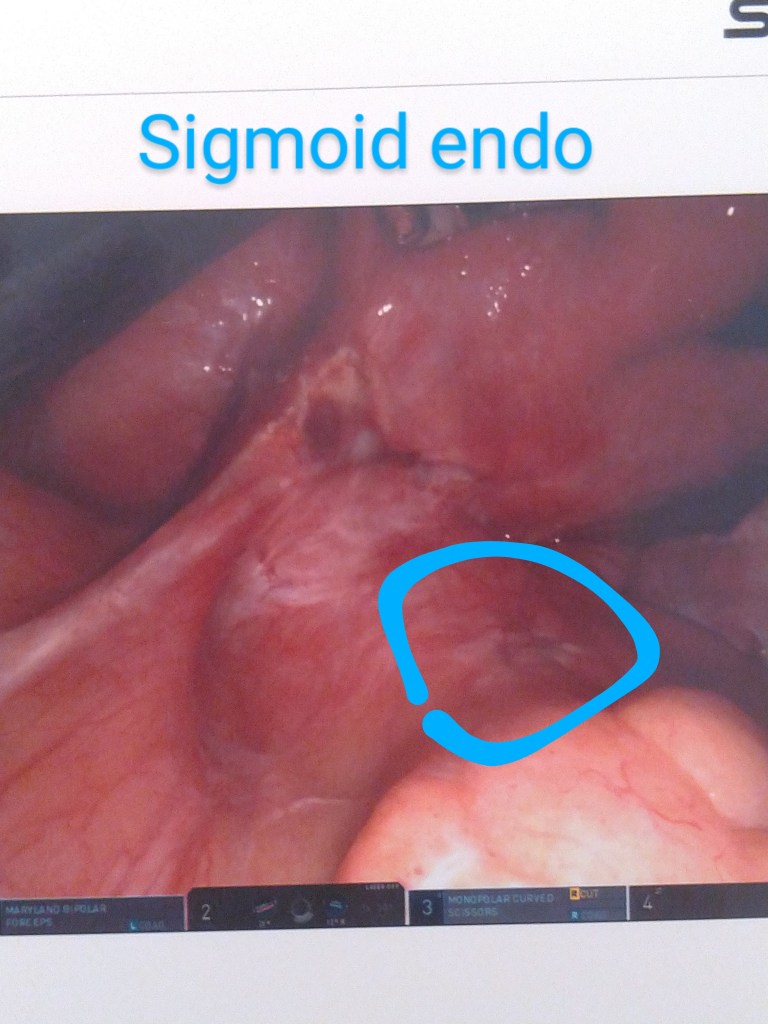
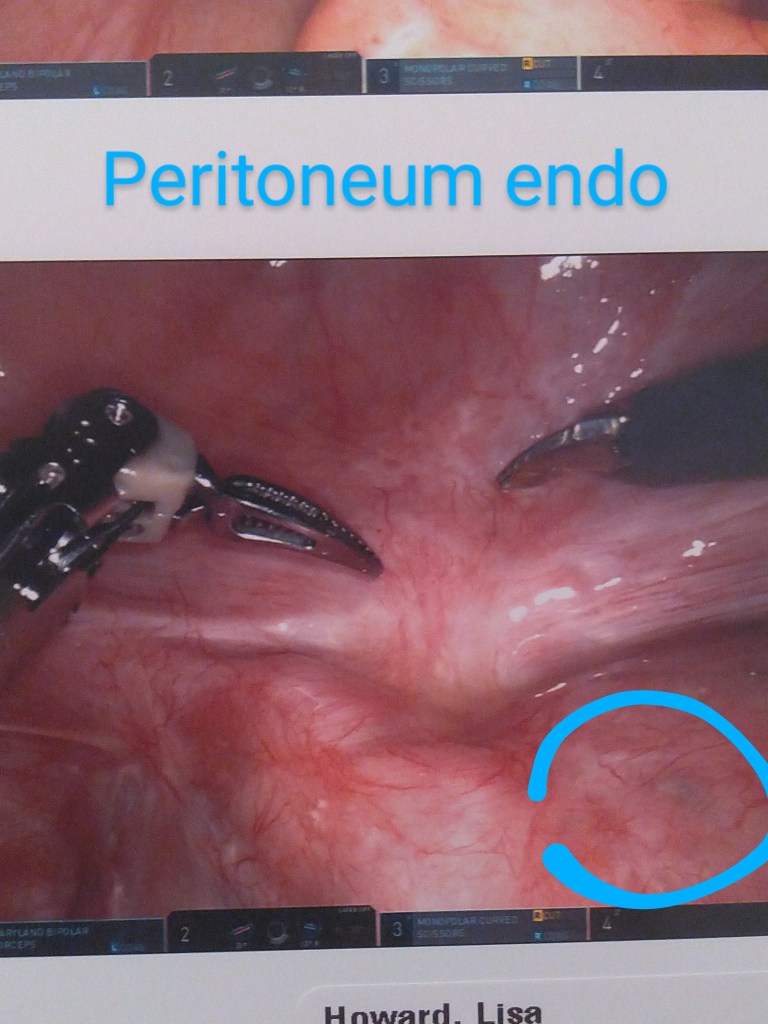
Surgery Photographs
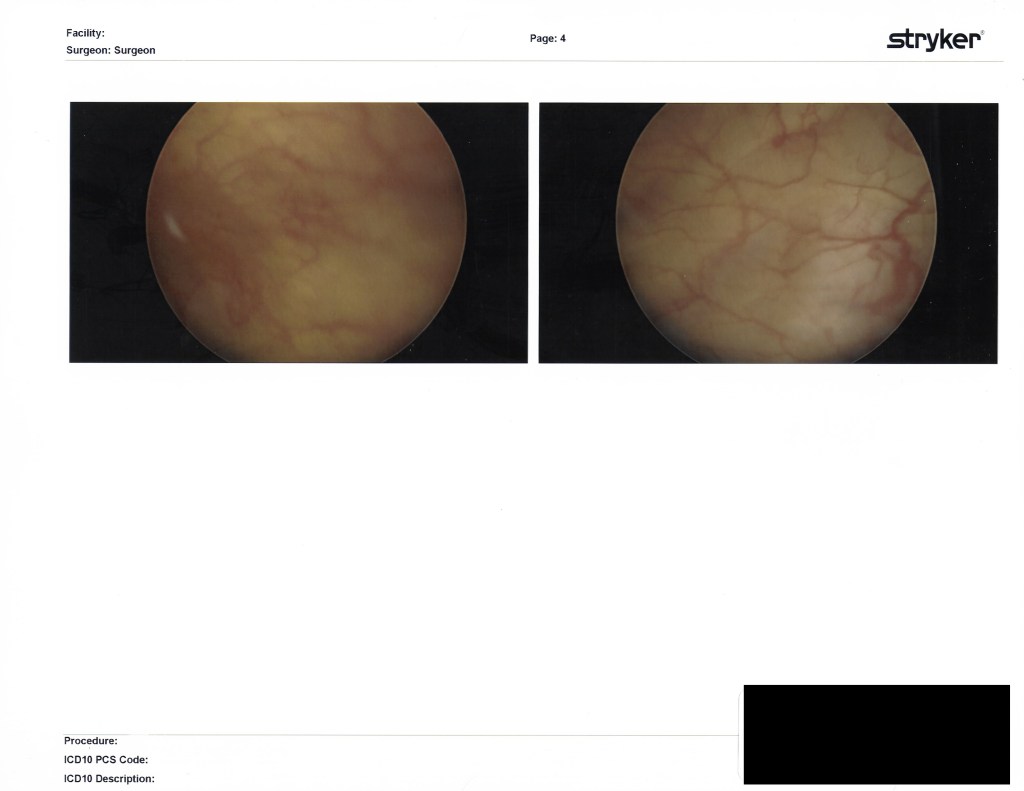
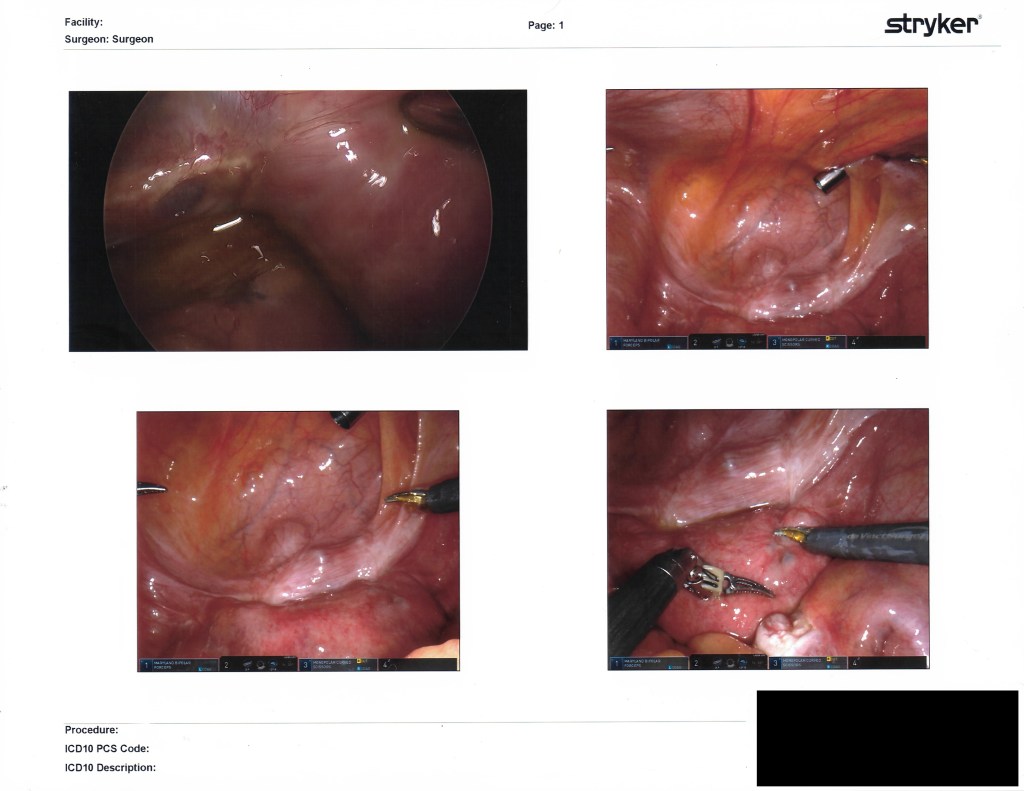
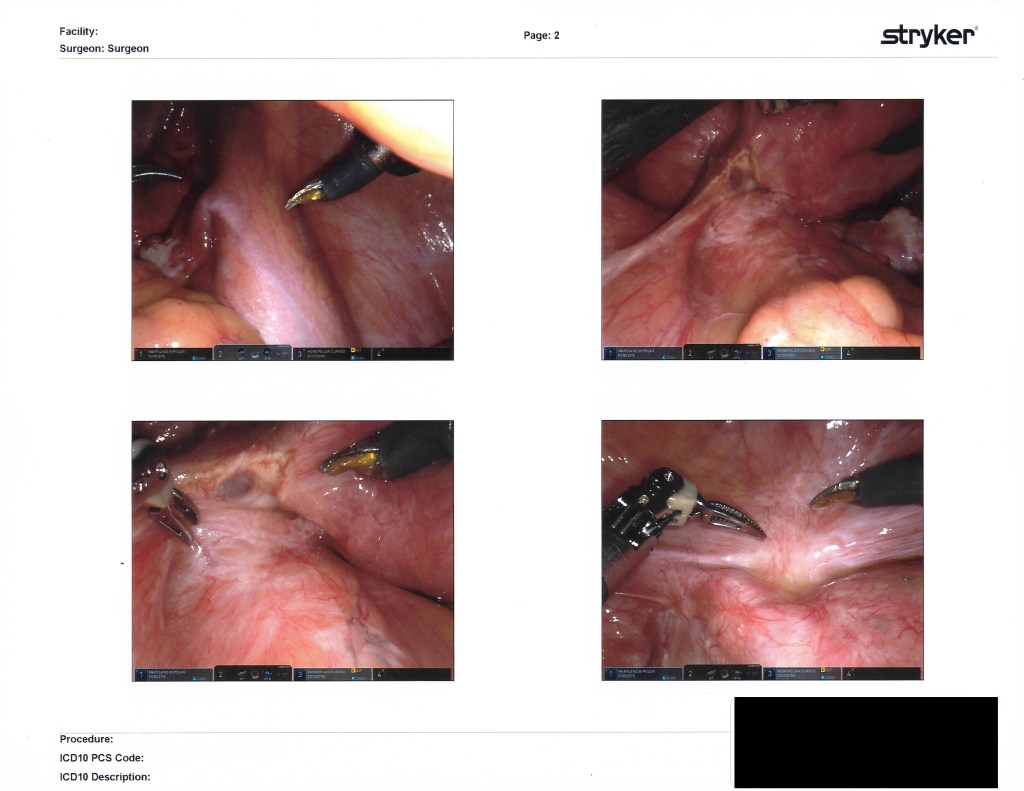
I’ve labeled these as best I could remember right after I left my post-op examination with Dr. Kurtulus. Enjoy the insides!!
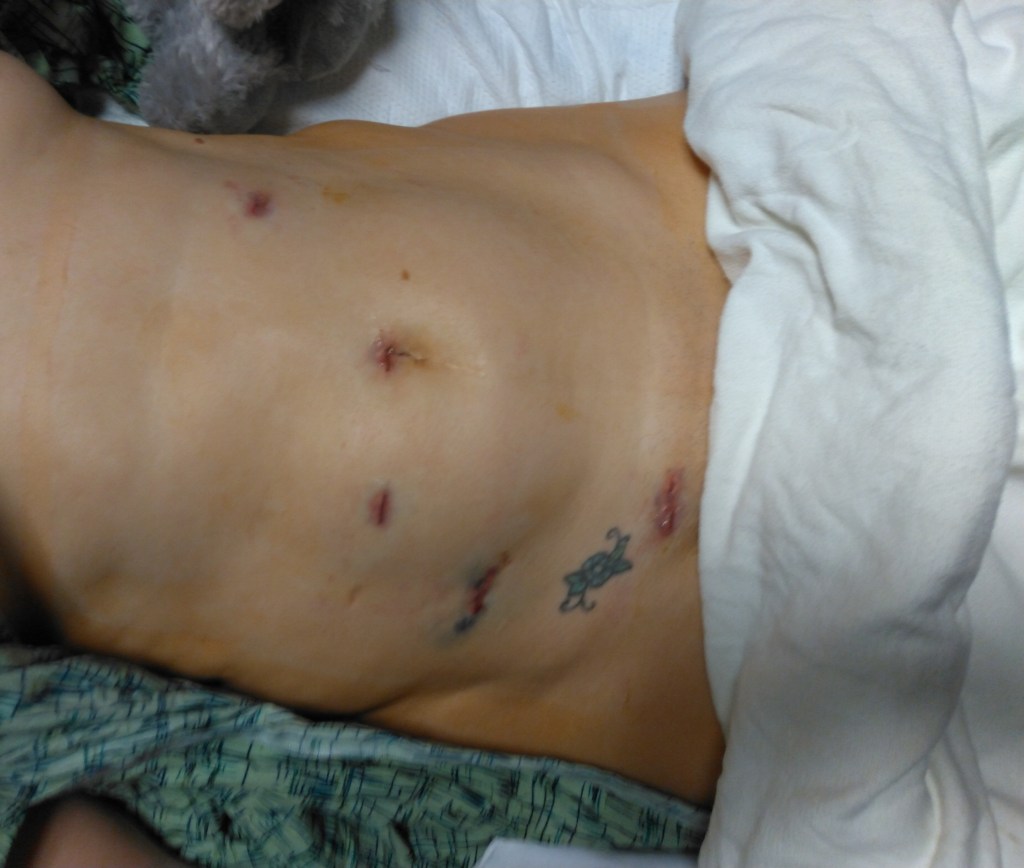
Recovery Photographs
And here’s a few fun photos I took during my recovery.

Hurtin’, but grateful for Mr. Victorious 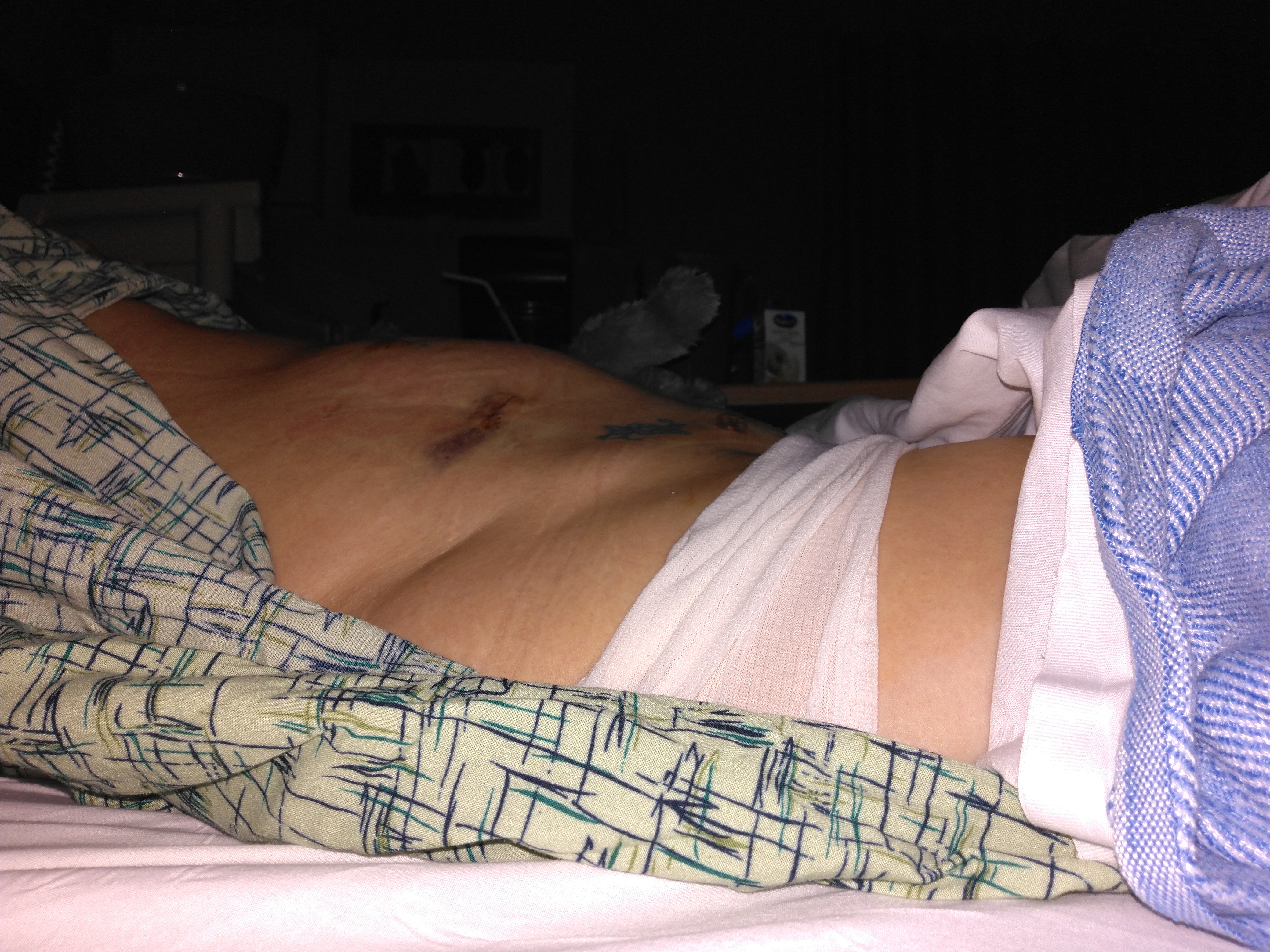
The side view 
I fell in love with this lighting. 
I GET TO ORDER FOOD! 
Salmon & ‘taters 
Bon Appétit! 
This was my last day! 
Mr. V is ready to go! 
THE GREAT ESCAPE! 
hehe Blue Cap! 
Rosie & I are home! 
Gutsy pillow from friends 
Home with my Hubby ❤ 
A gift for a friend ❤ 
Nurse Midnight
If you’d like to see how my incisions healed after one month, check out this li’l video I put together:
I am so very grateful to my surgeons, their office staff, all of the hospital staff, my husband, my friends, my family, and all of you for all of the expertise, support, prayers, and well-wishes!
*Updated December 9, 2020*
~ Again, I am a layman. I do not hold any college degrees, nor mastery of knowledge. Please take what I say with a grain of salt. If curious, do your own research. Validate my writings. Or challenge them. And ALWAYS feel free to consult with your physician. Always. Yours ~ Lisa


















Wishing you well my friend and thank you for such a detailed report of how you’ve been and raising awareness as always on a mostly unknown invisible illness. You’ve been through it but did they give you any indication wether this surgery will stop or slow down the growth??
Whatever the outcome you’re Amazing. Sending love to you 💛
LikeLiked by 1 person
Thank you so much! The usual speech I’ve received after my other surgeries: “We’ve removed all the Endometriosis that we could see (and he’s very thorough looking multiple times around the entire pelvic cavity). Hopefully it will not return.” I can only hold onto hope ❤ As of right now, I've got zero visible Endo inside me. BUT…I've also had microscopic Endometriosis discovered in past surgeries, so who knows what the body is doing ❤ Holding onto hope and a positive attitude
LikeLiked by 1 person
It is a journey. Why we go on this difficult, painful journey I know not but a better person we emerge.
Life life to its fullest, tell your story to help others and I hope you are pain free and under control for as long as you can be x
LikeLiked by 1 person
Wow. My goodness, you’ve been through so much… and to be in surgery during COVID on top of everything. Endo Warrior, indeed!
LikeLiked by 1 person